Why did I not report on Moderna results – here is a very well written response – https://www.independent.co.uk/voices/coronavirus-vaccine-covid-19-cure-doctor-moderna-novavax-oxford-a9523091.html
“77 percent of vaccines for infectious diseases make it through Phase I, but only 33 percent make it through the entire process overall.”
“45 patients who received the vaccine, the data on “neutralising antibody data are available only for the first four participants in each of the 25-microgram and 100-microgram dose level cohorts.” In other words, that means that when it comes to finding out whether the vaccine elicits an antibody response that could potentially fight the coronavirus, they only had data on eight patients.”
“the only data Moderna alluded to were from mice. Not only are there huge differences between mice and men, but history also proves that success in animal models is often not replicated in human studies. This is especially the case for Moderna’s messenger RNA vaccine, which would be the world’s first to ever reach the market if it passes clinical trials.”
“In many ways, the vaccine almost behaves like an RNA virus itself except that it hijacks your cells to produce the parts of the virus, like the spike protein, rather than the whole virus. Some messenger RNA vaccines are even self-amplifying. That means they encode not only the protein antigen of interest to elicit an immune response but also produce their own RNA dependent RNA polymerase, so that they can force the cell to replicate more copies of it. At that point, it will be hard to convince conspiracy theorists and anti-vaxxers that a self-amplifying messenger RNA vaccine is not an artificially created self-replicating virus. In fact, public acceptance of this new paradigm is not something to be easily dismissed nor taken for granted. There are unique and unknown risks to messenger RNA vaccines, including the possibility that they generate strong type I interferon responses that could lead to inflammation and autoimmune conditions.”
“Let’s base our excitement and exuberance on the actual facts and evidence and data rather than our labile emotions and feelings. We are all in this together, and that includes poor people in America and poor people in poor countries around the world who deserve an eventual coronavirus vaccine that is safe, effective, and — last but not least — affordable.”
A US micro study – Arkansas Church event – https://www.cdc.gov/mmwr/volumes/69/wr/mm6920e2.htm?s_cid=mm6920e2_w
Nothing earth shattering that the other micro studies didn’t note. Indoor prolong gathering with likely simple ventilation – very unfortunate they didn’t delve into this – is not a good decision to protect against infection. Indoors poor ventilation creates a perfect breeding ground for the virus.
“Among 92 attendees at a rural Arkansas church during March 6–11, 35 (38%) developed laboratory-confirmed COVID-19, and three persons died. Highest attack rates were in persons aged 19–64 years (59%) and ≥65 years (50%). An additional 26 cases linked to the church occurred in the community, including one death.”
“as of April 22, 61 confirmed cases (including eight [13%] hospitalizations and four [7%] deaths) had been identified in persons directly and indirectly associated with church A events.”
The conclusion shouldn’t be to end practices like this – it should be to question how to make it better. How to make it like a 14 hour flight so no one gets impacted (yesterday note). I suspect this can be solved with a modern fresh air HVAC unit with UV filtration system AND better practice of social distancing and wearing mask.
Another antibody test indicating infection rate of general public 4% – LA County – https://jamanetwork.com/journals/jama/fullarticle/2766367
“In this community seroprevalence study in Los Angeles County, the prevalence of antibodies to SARS-CoV-2 was 4.65%. The estimate implies that approximately 367 000 adults had SARS-CoV-2 antibodies, which is substantially greater than the 8430 cumulative number of confirmed infections in the county on April 10.3 Therefore, fatality rates based on confirmed cases may be higher than rates based on number of infections. In addition, contact tracing methods to limit the spread of infection will face considerable challenges.”
The percentage is too high to think you can contain it is the perspective I have been having for quite some time. The prevalence means Sweden approach may be the wises in the long run unless we come up with a treatment plan or vaccine in less than 6 months.
When will the media learn to not jump on subject matters they know little about or at the VERY LEAST just report don’t add bias…. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7162746/
Reporting FDA says a drug could be harmful is not reporting – ALL drugs even vitamins can be harmful – it’s the probability of harm they should note – that’s reporting….
Will they apologize for delaying research or causing deaths which perhaps could be preventive? AND for what to make fun of a person they don’t like – why be so childish and promote a person you don’t like?
“We implemented PEP with HCQ safely under proper monitoring and no patients were diagnosed with COVID-19 additionally. Randomized clinical studies are needed to evaluate if PEP is an effective option for outbreak response against COVID-19 in LTCHs.”
“Long-term care hospitals (LTCHs) are vulnerable to cluster outbreaks. Because patients in LTCHs need continuous intimate cares, it is difficult to find facilities and healthcare personnel for their separate isolation care in a large outbreak situation. Furthermore, they are the risk group if infected. Although several drugs have been proposed as treatment regimens, there are no data on the effectiveness and safety of post-exposure prophylaxis (PEP) for COVID-19. On February 23, a hospital social worker at a LTCH in Busan was diagnosed with COVID-19 after attending a religious service of Shincheonji 7 days earlier and inpatients and hospital staff were exposed to her. We are sharing our experience of the outbreak response in the LTCH including PEP using hydroxychloroquine (HCQ).”
“We started PEP with HCQ for patients and careworkers, on February 26 (Supplement Fig. 1). Physicians and pharmacists were educated about potential adverse events. HCQ was administrated orally at a dose of 400mg daily until the completion of 14 days of quarantine. A checklist for common adverse events was distributed (Supplement Fig. 2). The study was approved and informed consent was waived by the Institutional Review Board of Pusan National University Hospital (H-2003-014-089).”
“Postmortem PCR tests with URT specimens were performed for 2 patients who died during quarantine period and the results were negative. Two mortality cases, a 96 years old male and an 84 years old female with Alzheimer disease, had been receiving the end of life cares. For the remaining 191 patients and 121 hospital staff who had been tested negative first for COVID-19, follow-up PCR tests were conducted one or two days prior to discontinuing 2 week-period of quarantine and all were negative.”
Not to claim this as a solution for all – but to deny this option with generally a limited COST (both in terms of $ and adverse reaction) would be negligent. From Dr. Kory testimony – https://www.hsgac.senate.gov/imo/media/doc/Testimony-Kory-2020-05-06-REVISED.pdf:
“1- The Declaration of Geneva of the WMA binds the physician with the words, “The health of my
patient will be my first consideration,”
2- International Code of Medical Ethics declares that, “A physician shall act in the patient’s best
interest when providing medical care.”
3- Article 37 of the WMA declaration of Helsinki, titled: “Unproven Interventions in Clinical Practice”
It reads, and I paraphrase: “In the treatment of an individual patient, where proven interventions do
not exist, a physician may use an unproven intervention if in the physician’s judgement it offers hope
of saving life, re-establishing health or alleviating suffering.”
Wear the mask in social settings indoor…. https://fightcovid19.hku.hk/hku-hamster-research-shows-masks-effective-in-preventing-covid-19-transmission/
“In the first experiment, no surgical masks were placed between the two cages. In the second one, a surgical mask was placed closer to the healthy hamsters. In the third experiment, the mask was placed closer to the infected, as if the healthy ones or the infected were wearing masks.
With no partition in between the cages, two-thirds of the healthy hamsters were infected a week later. In the following two experiments with masks in between, the infection rates were lowered to one-third and one-sixth respectively.”
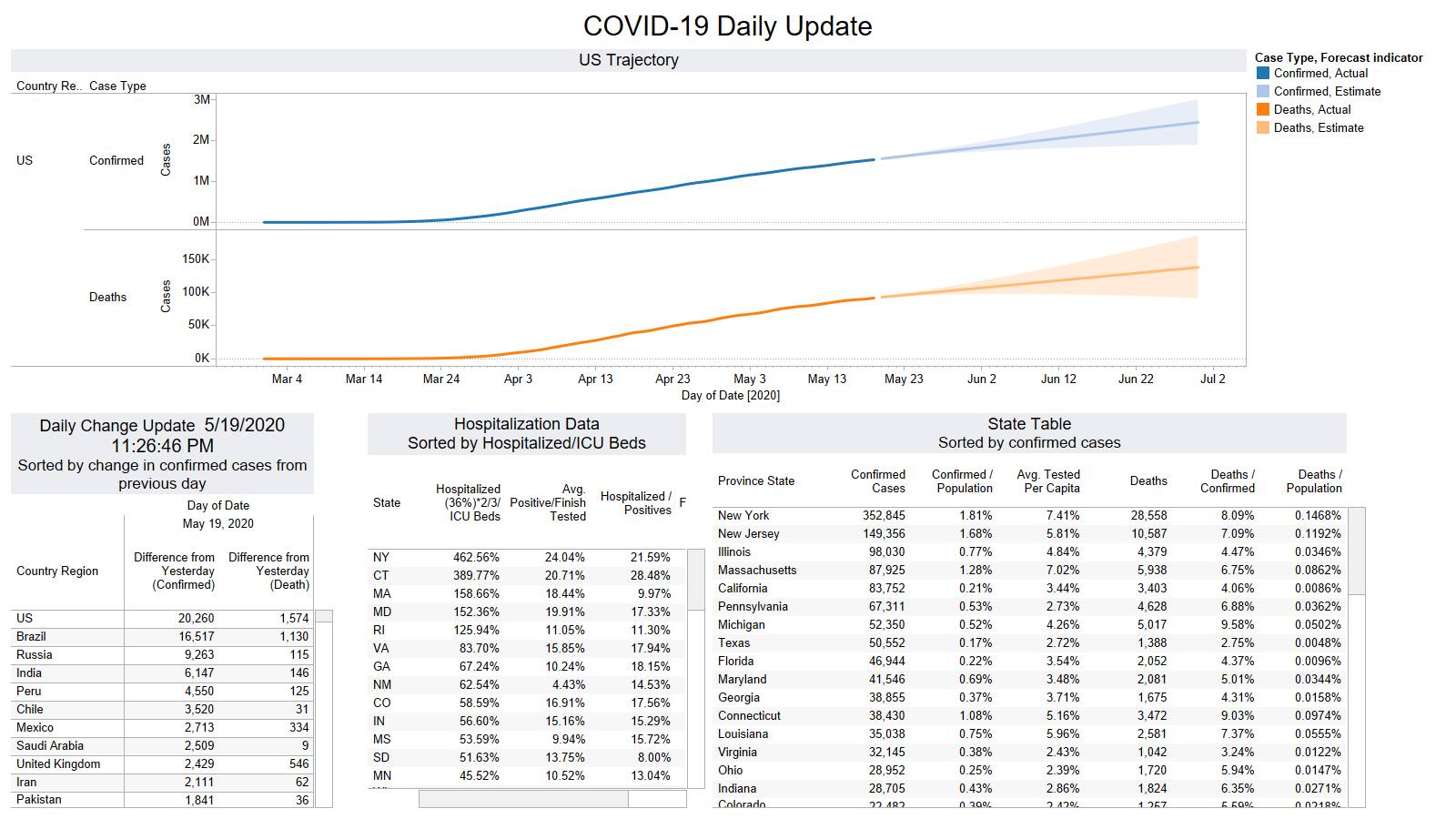
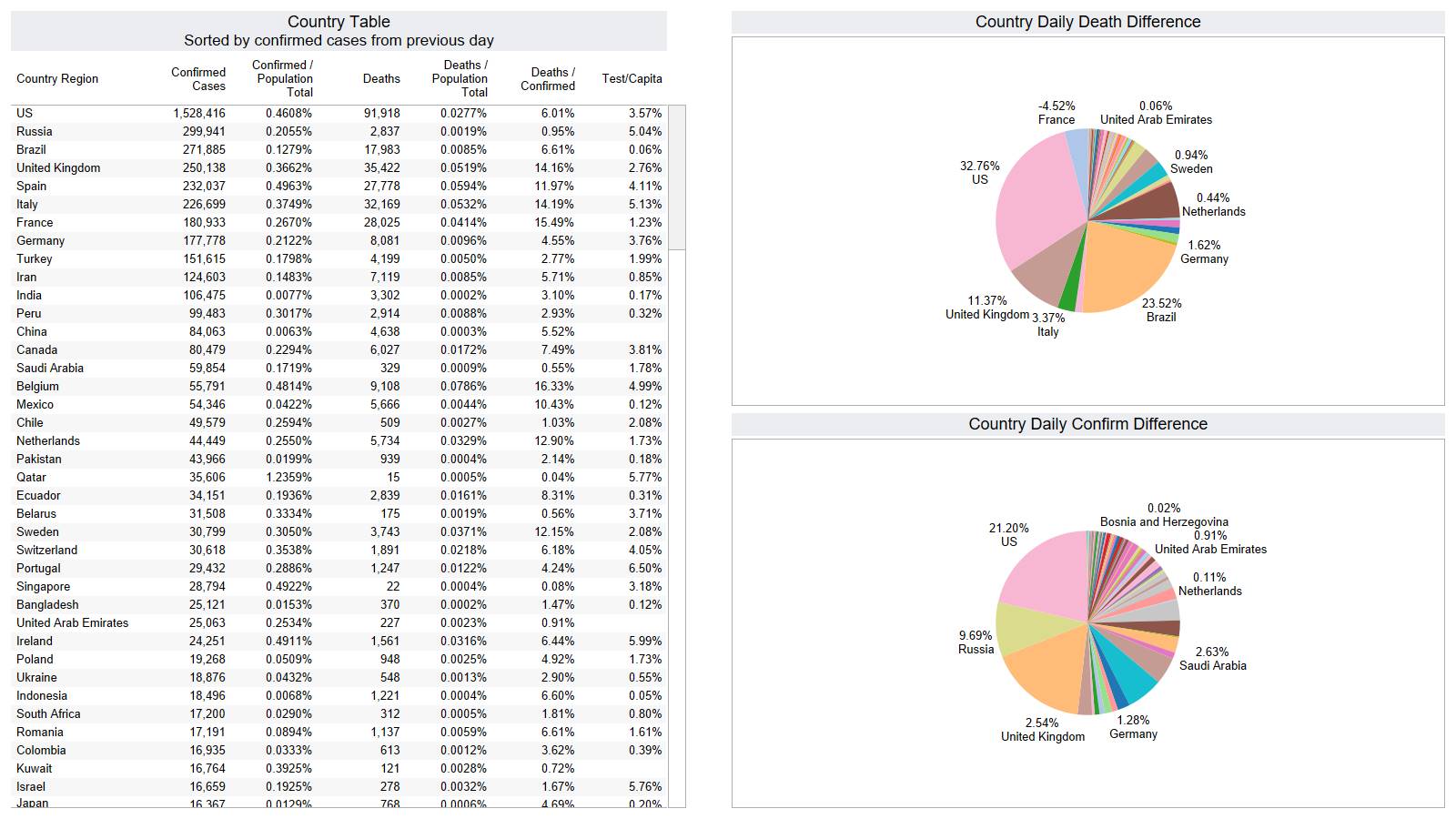
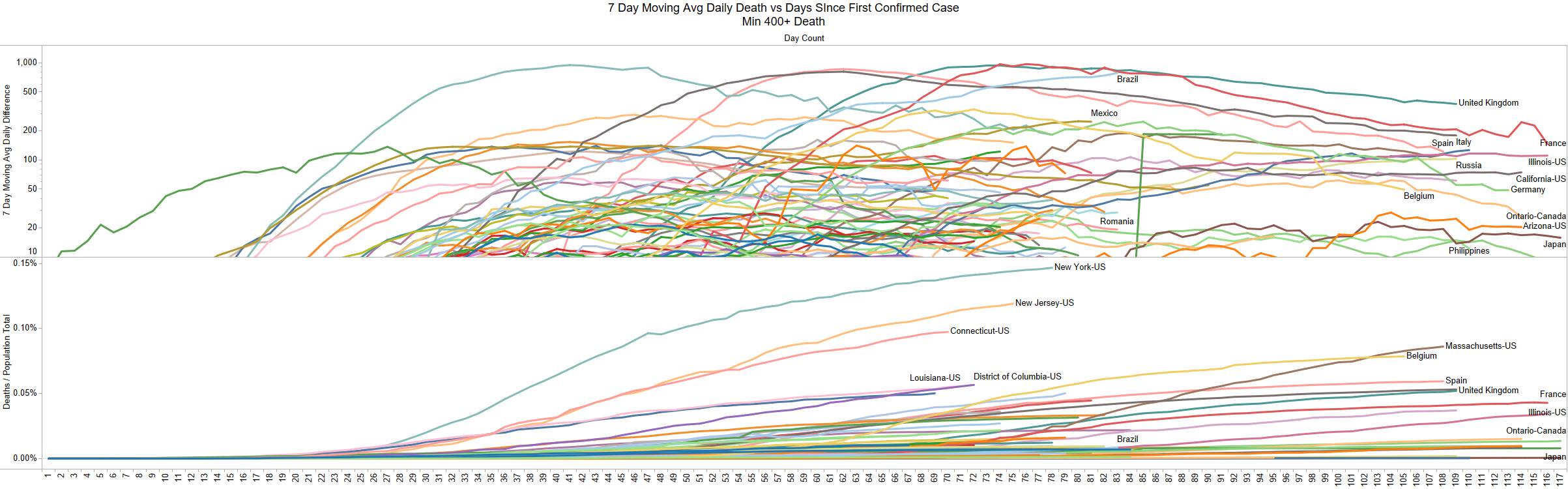
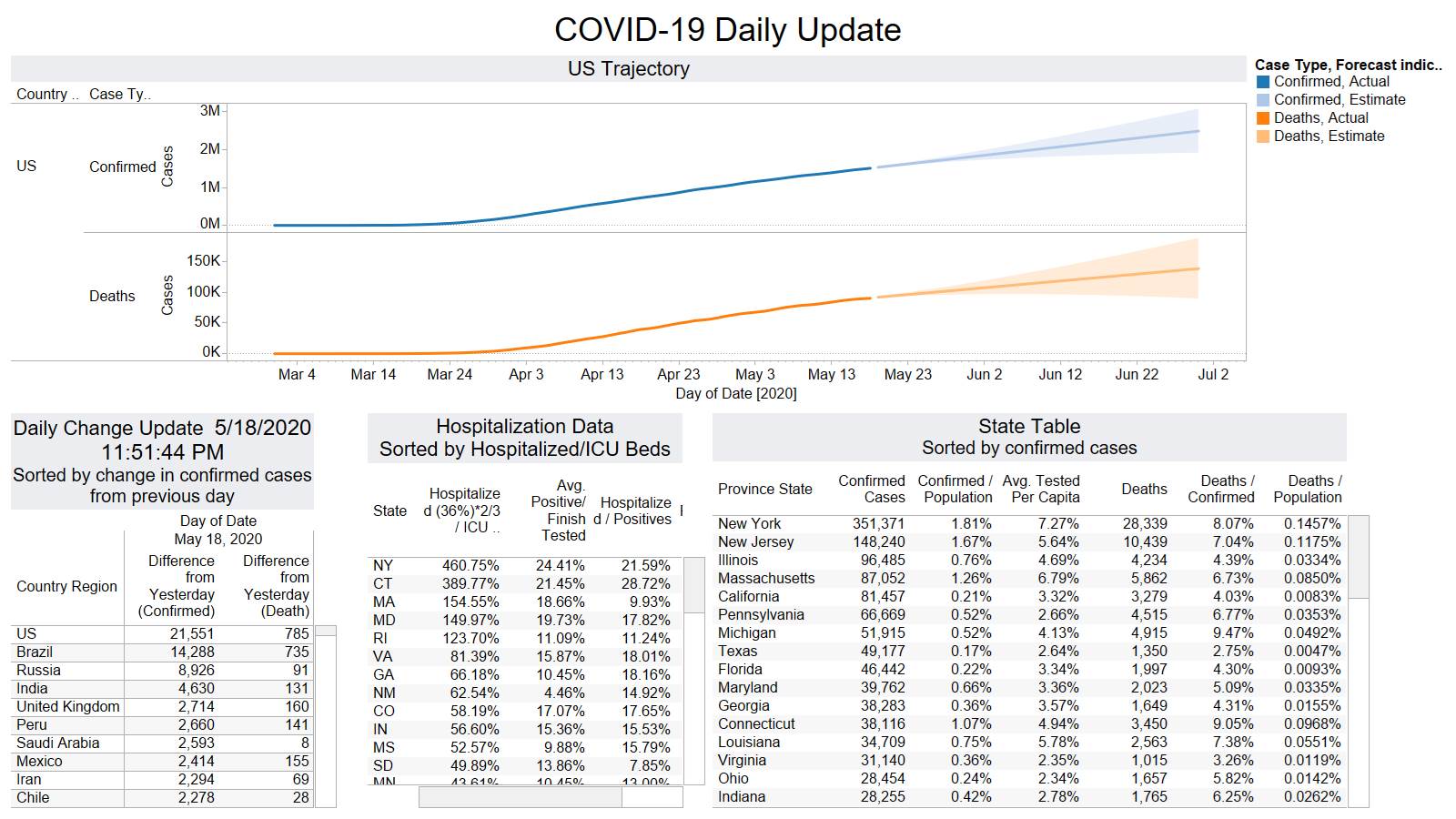
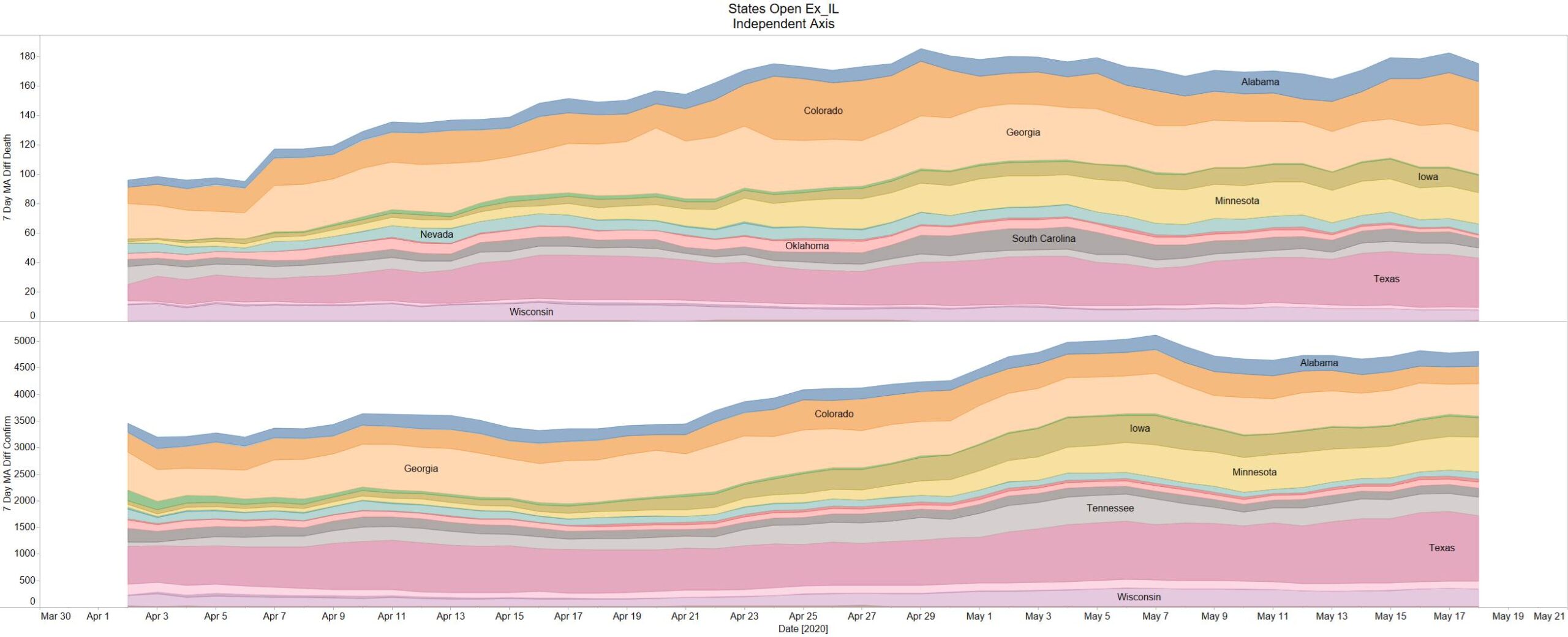
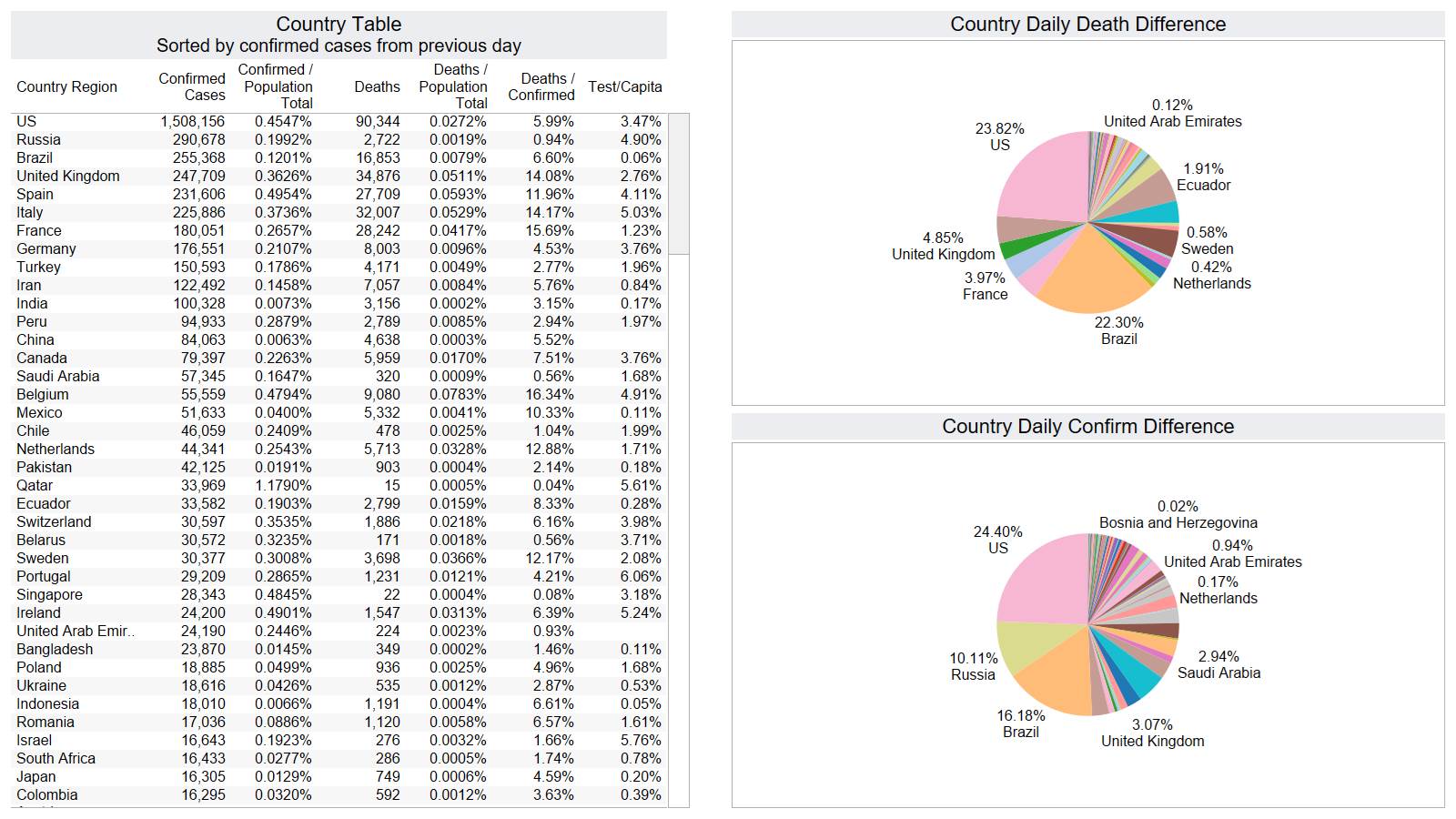
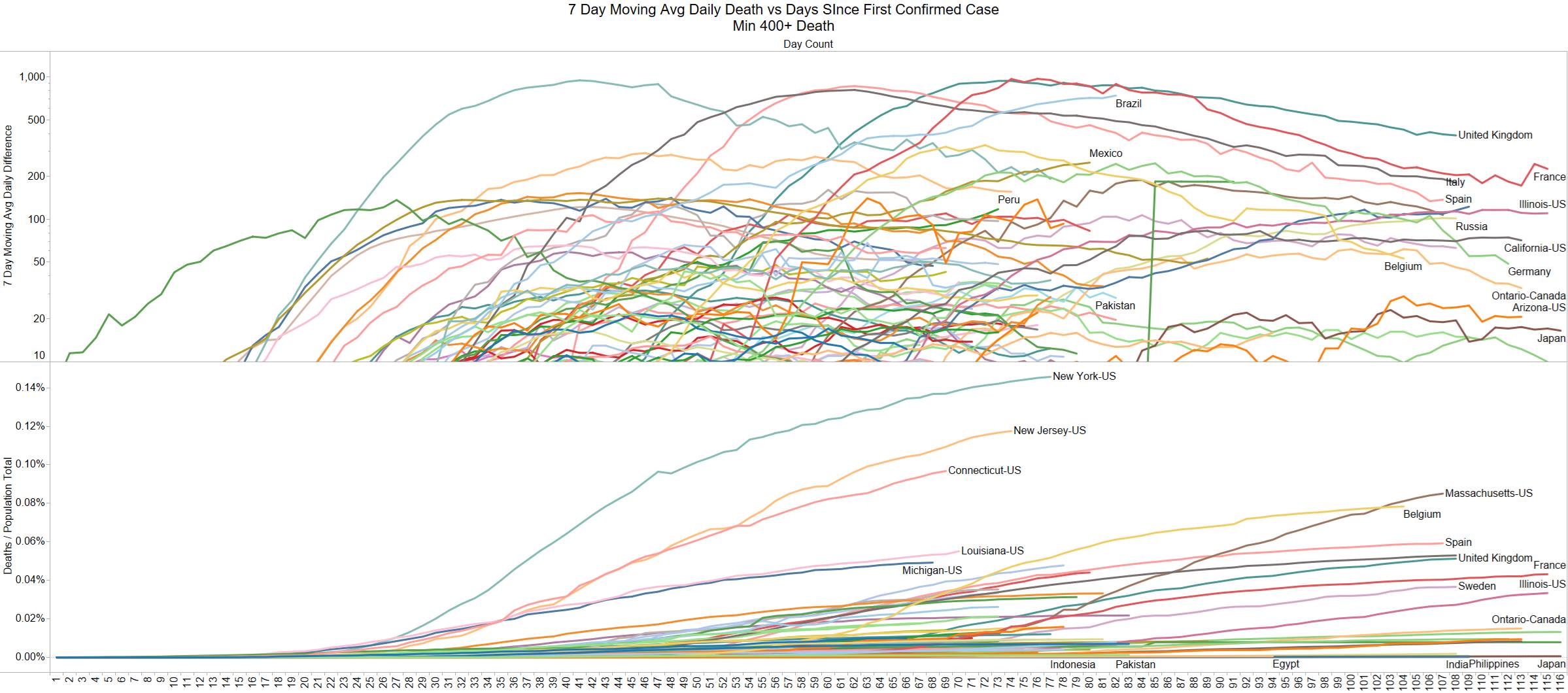
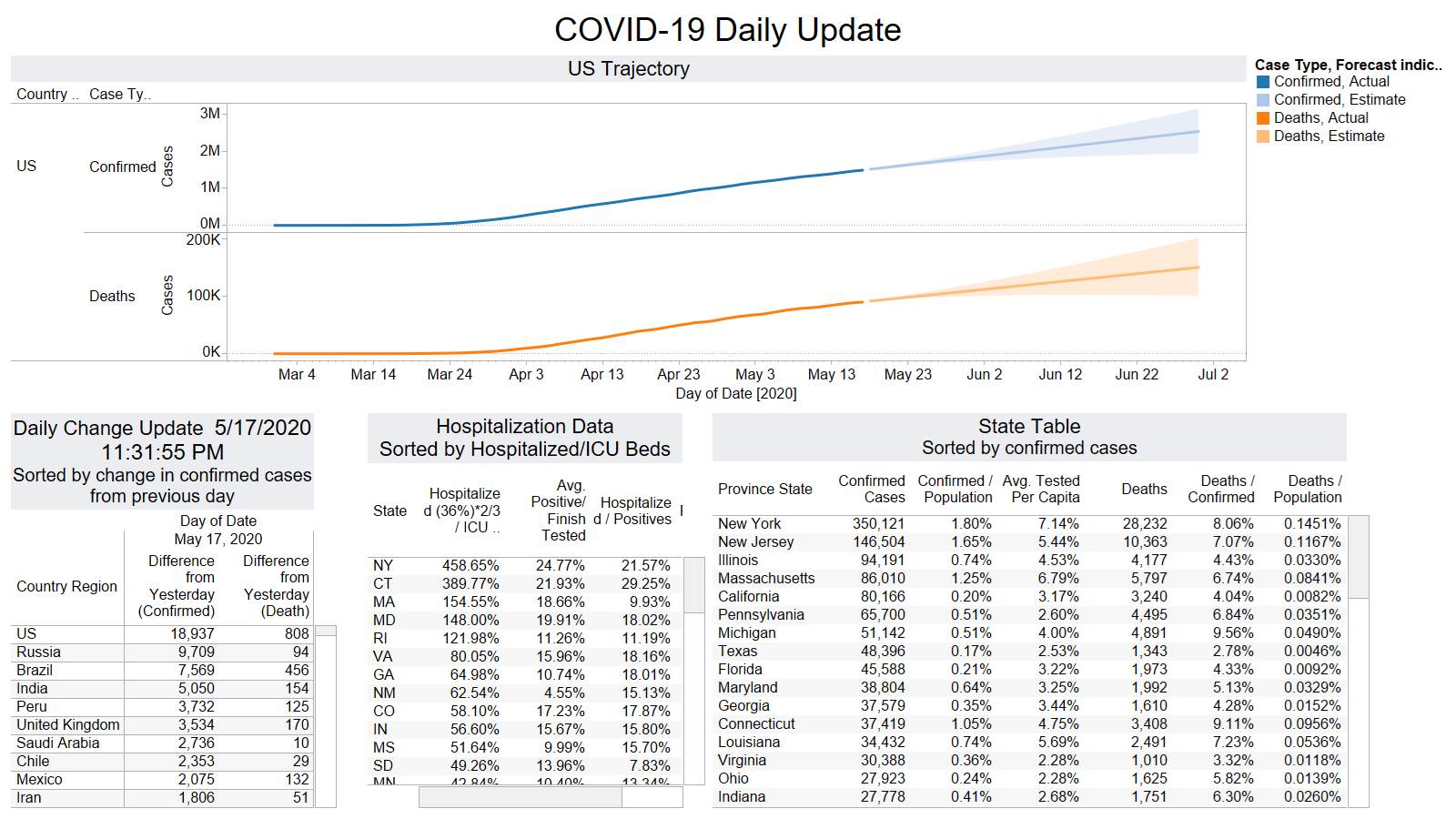
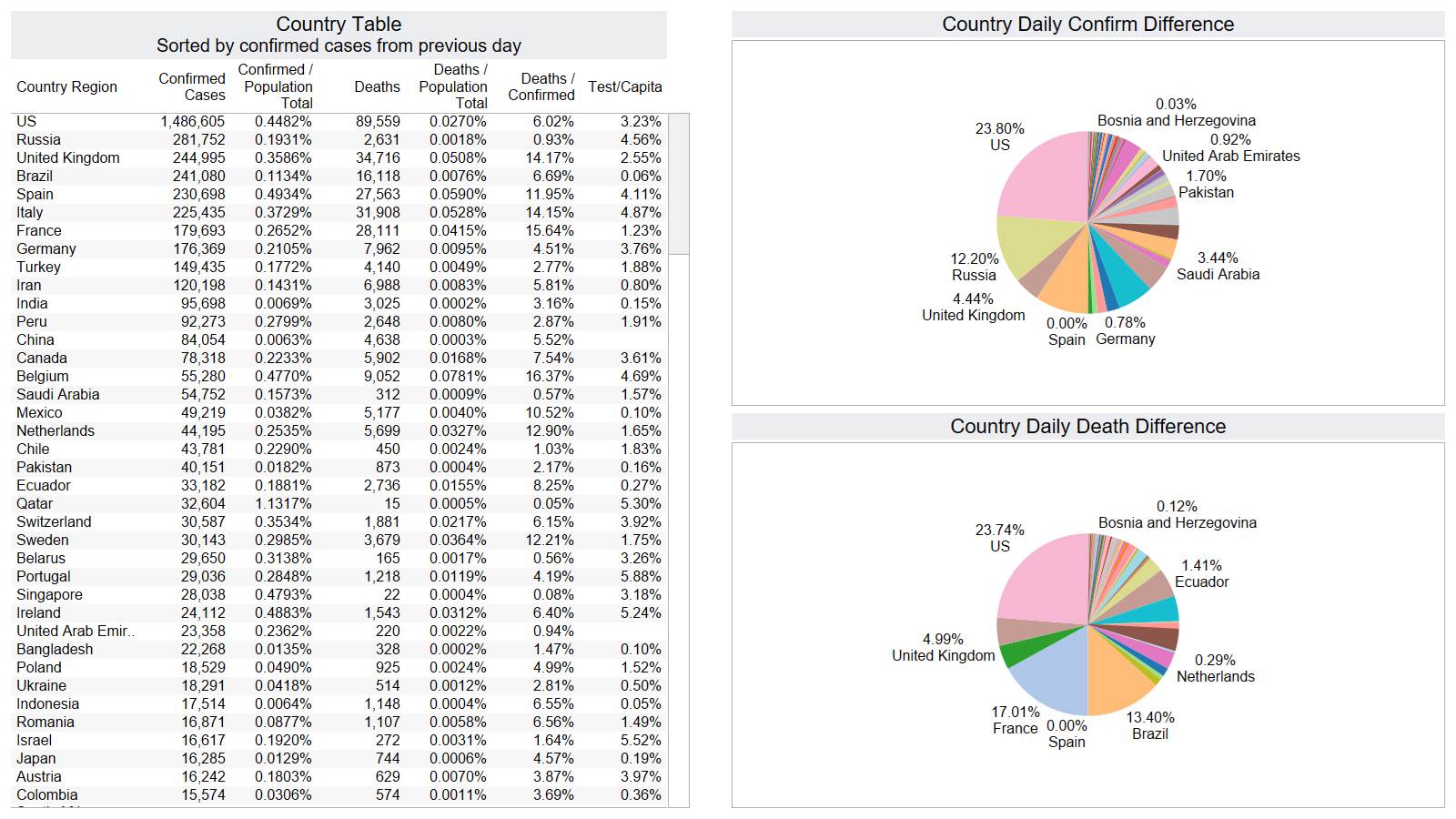
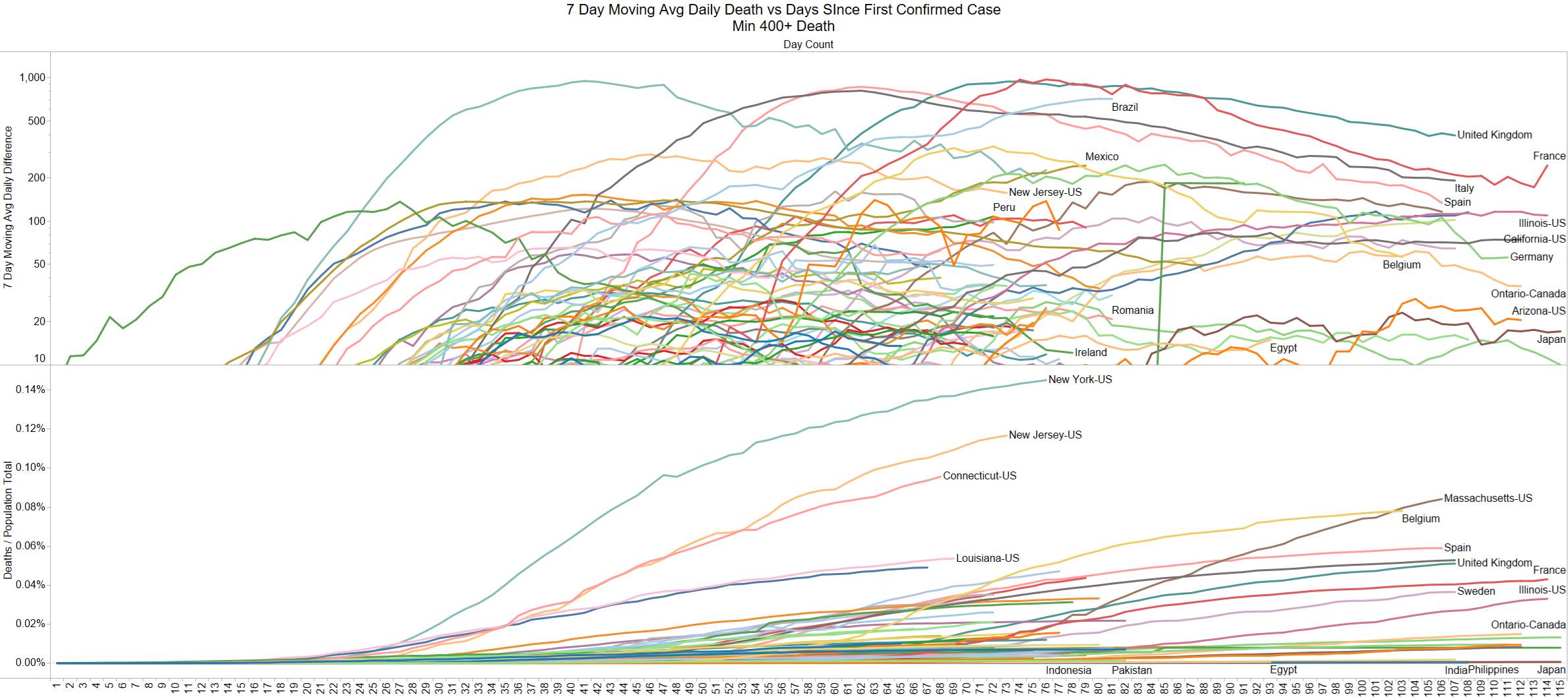
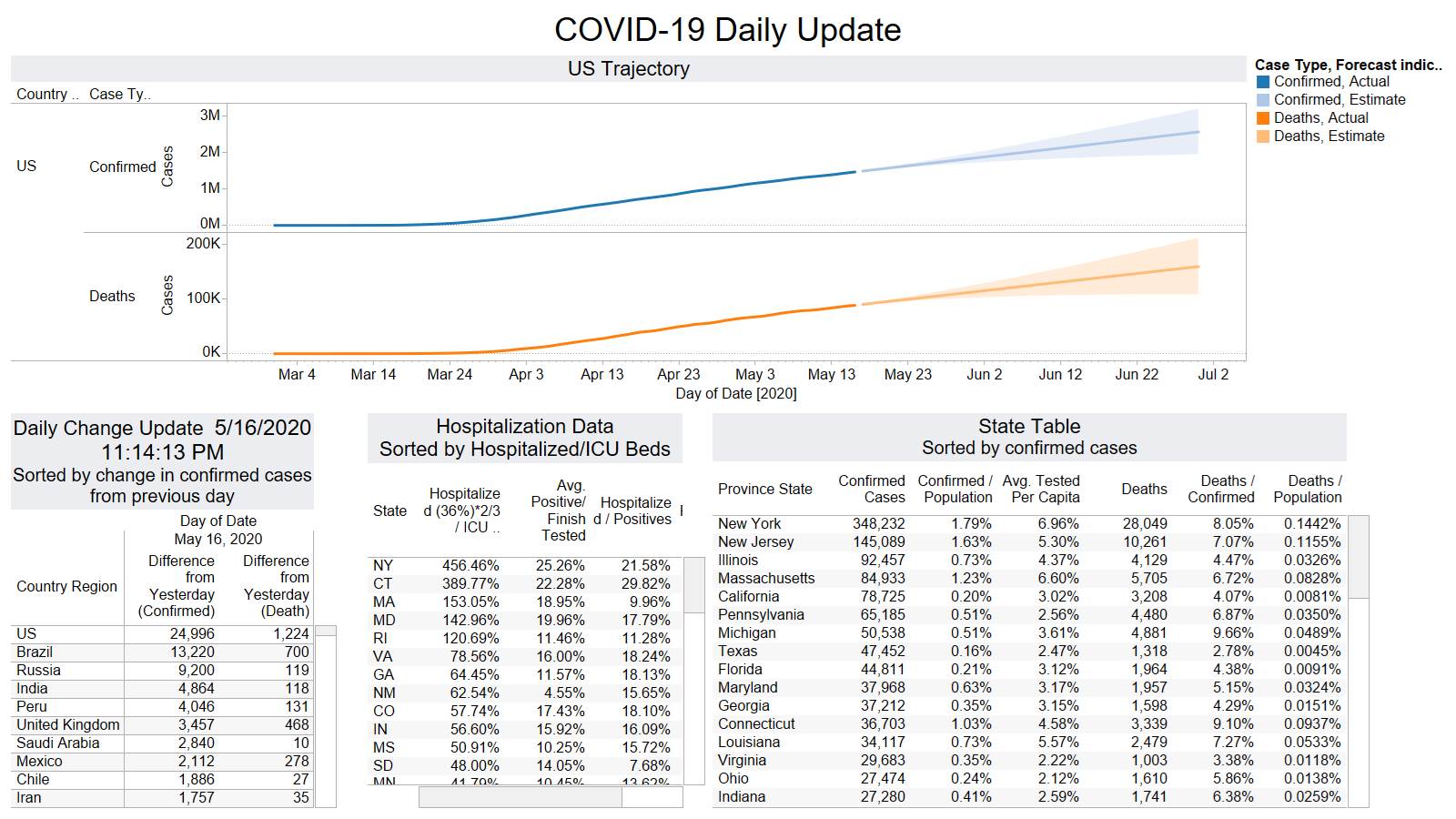
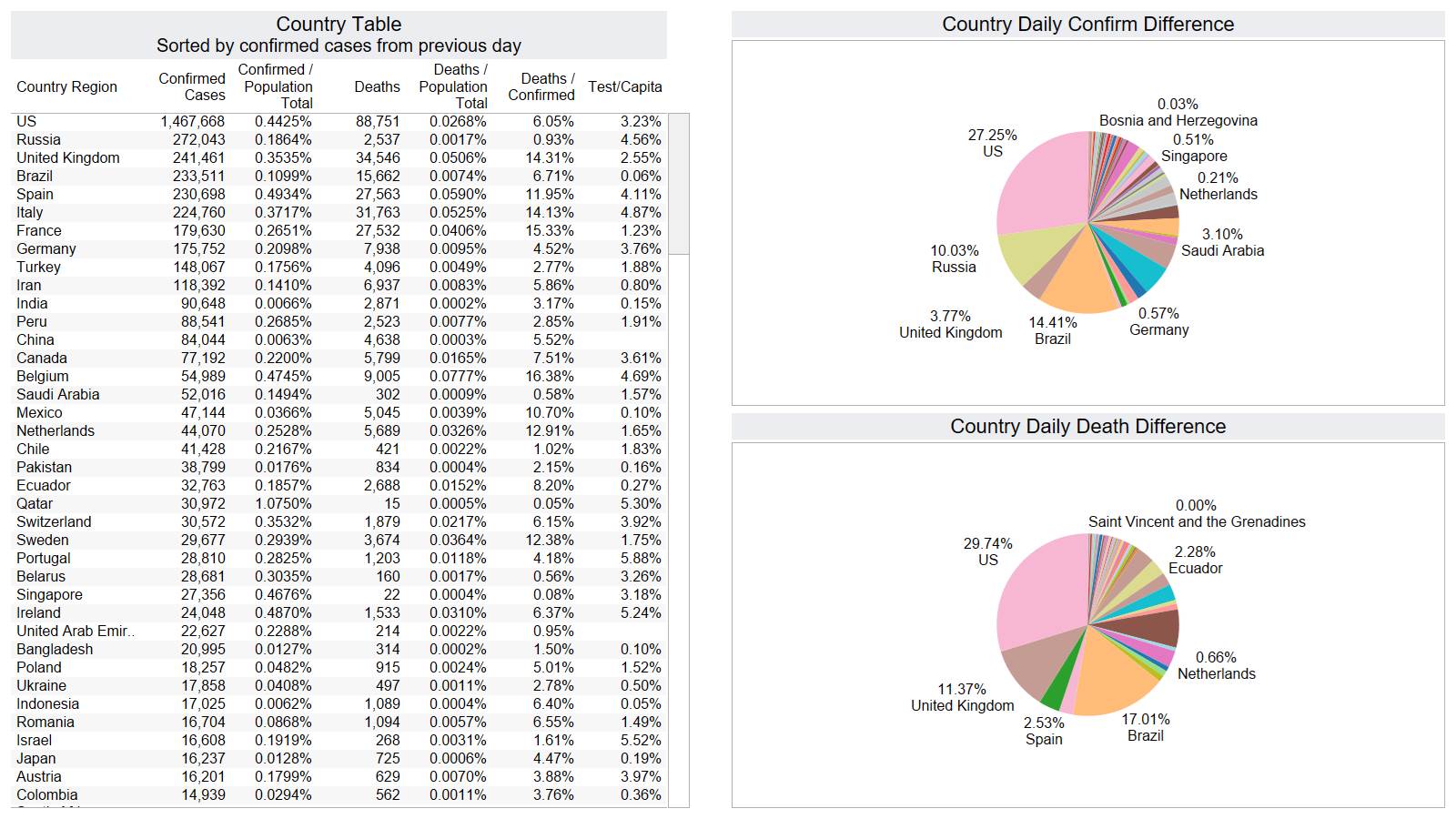
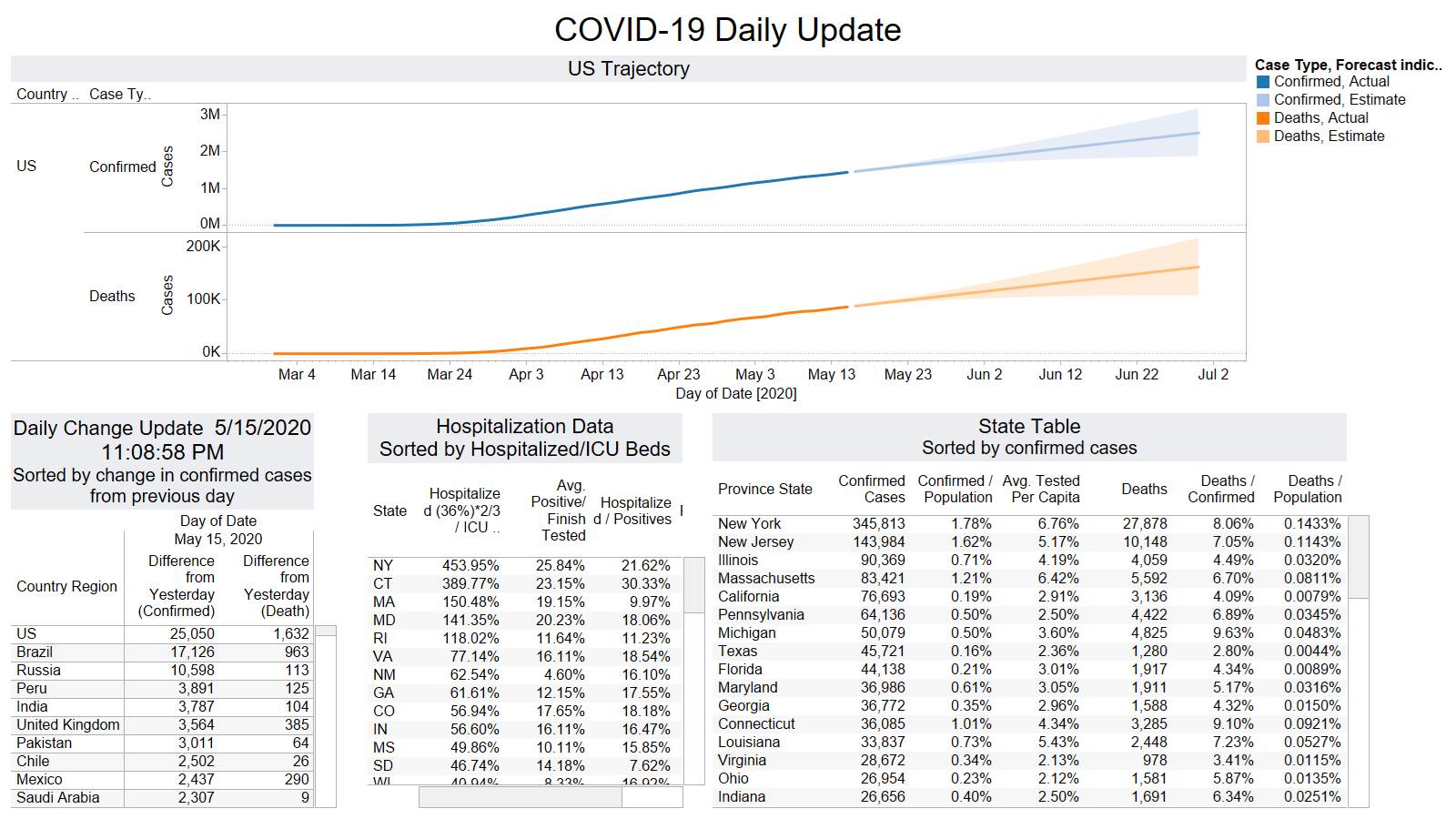
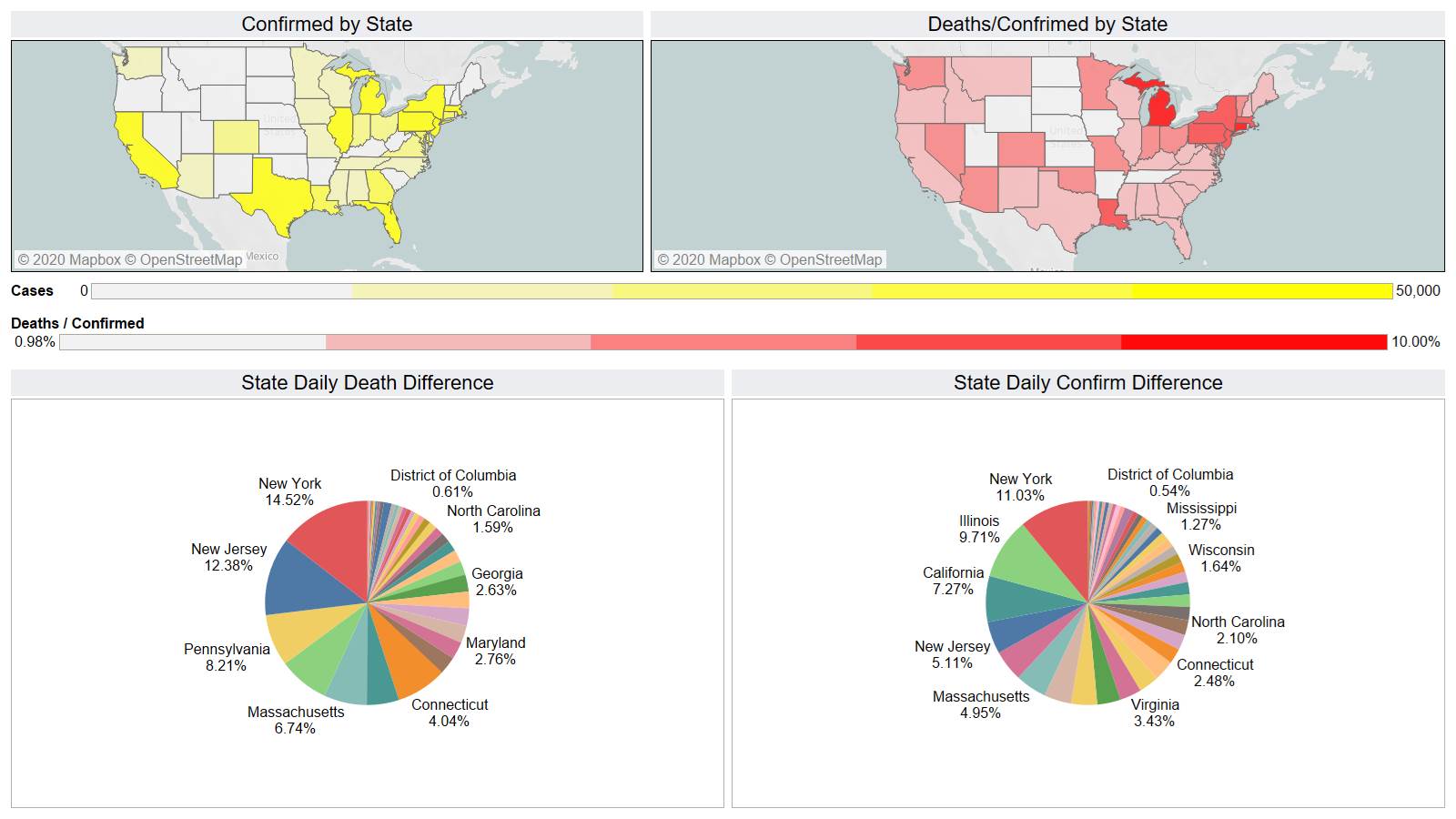
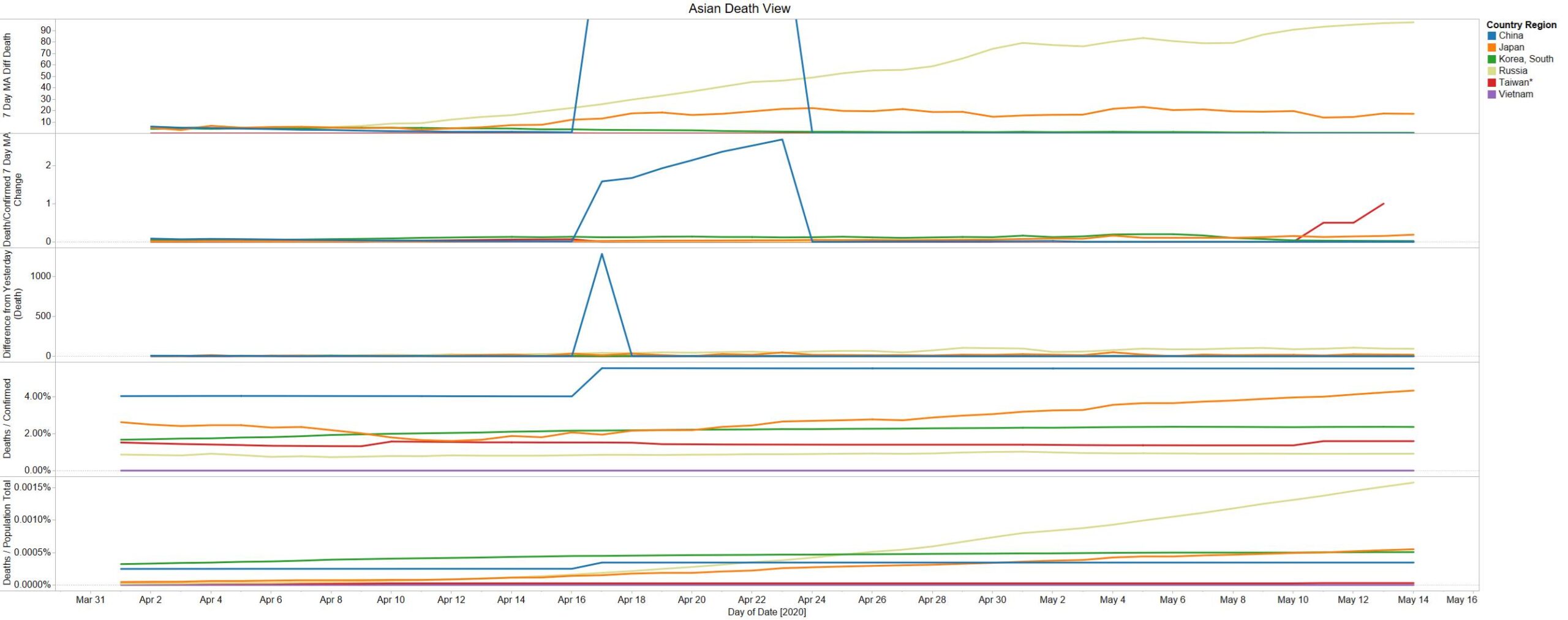
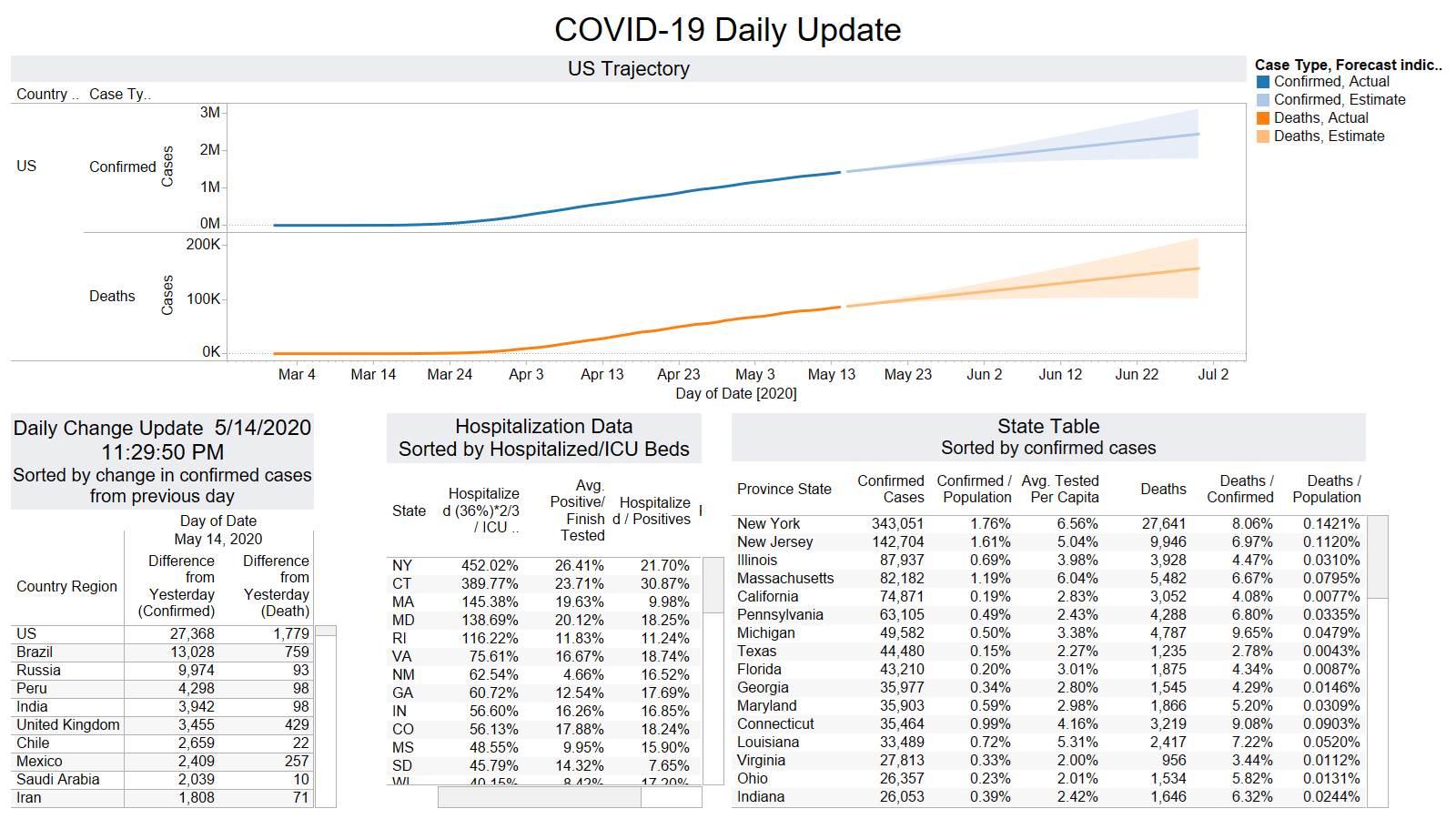
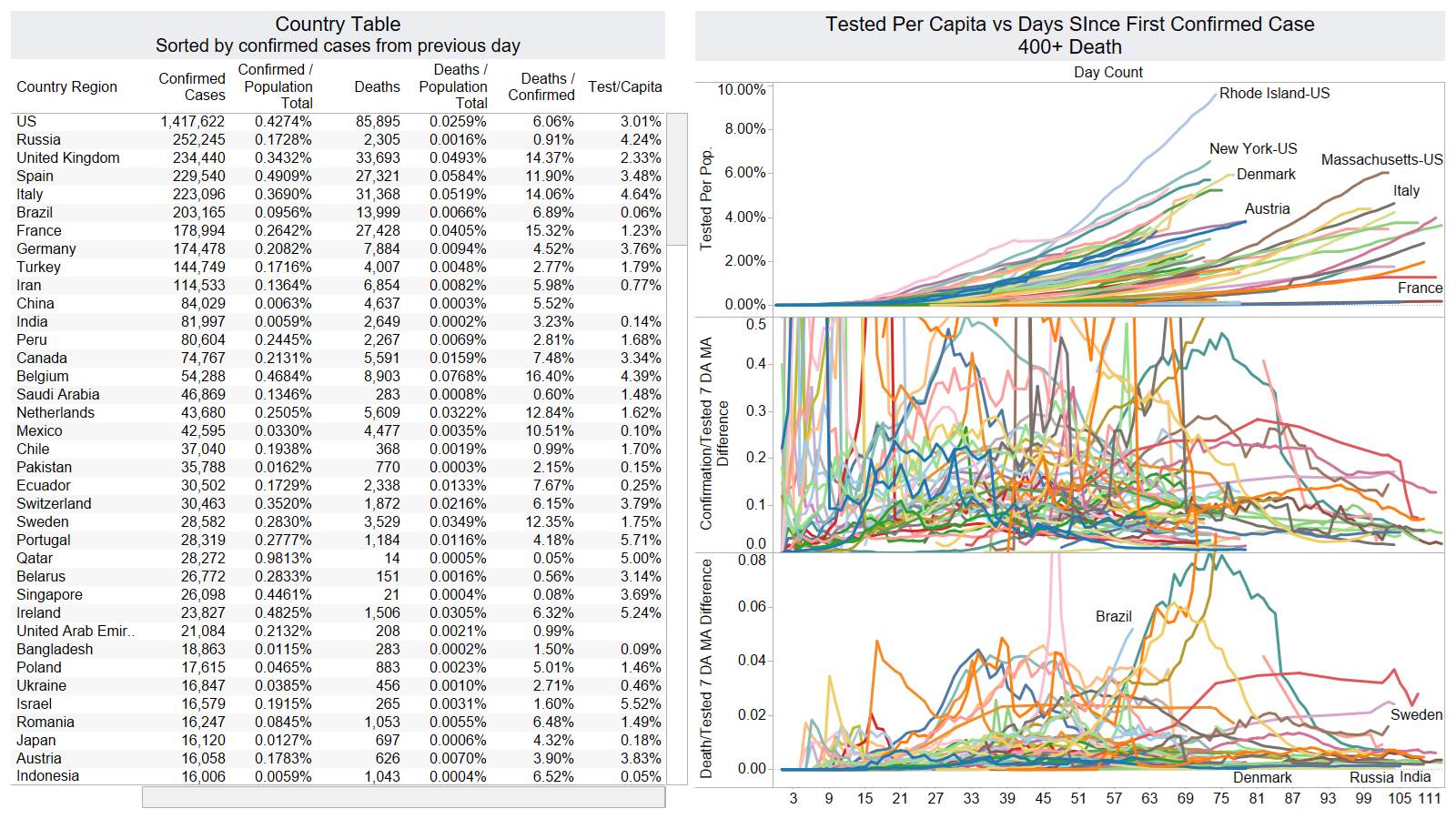
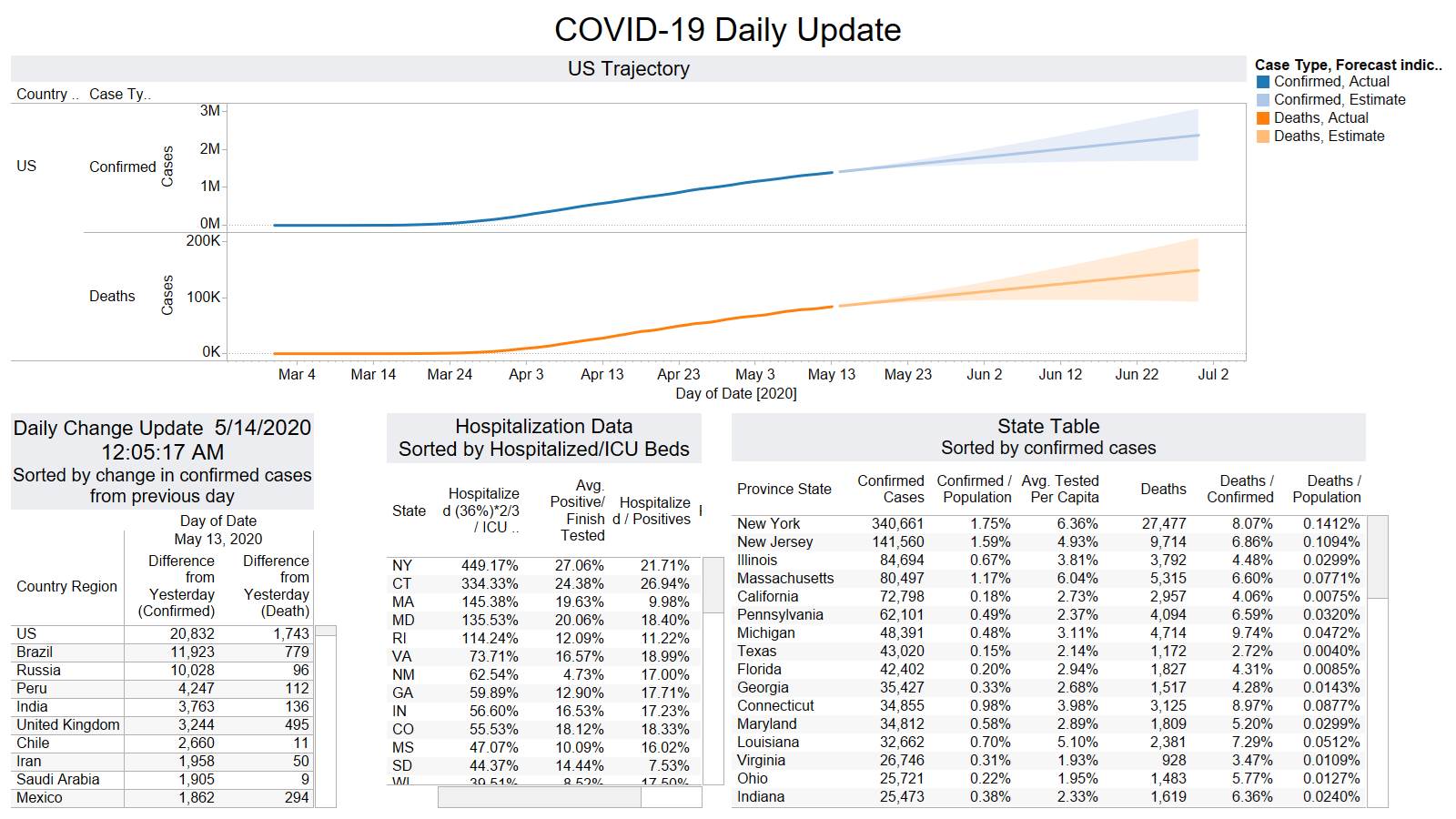
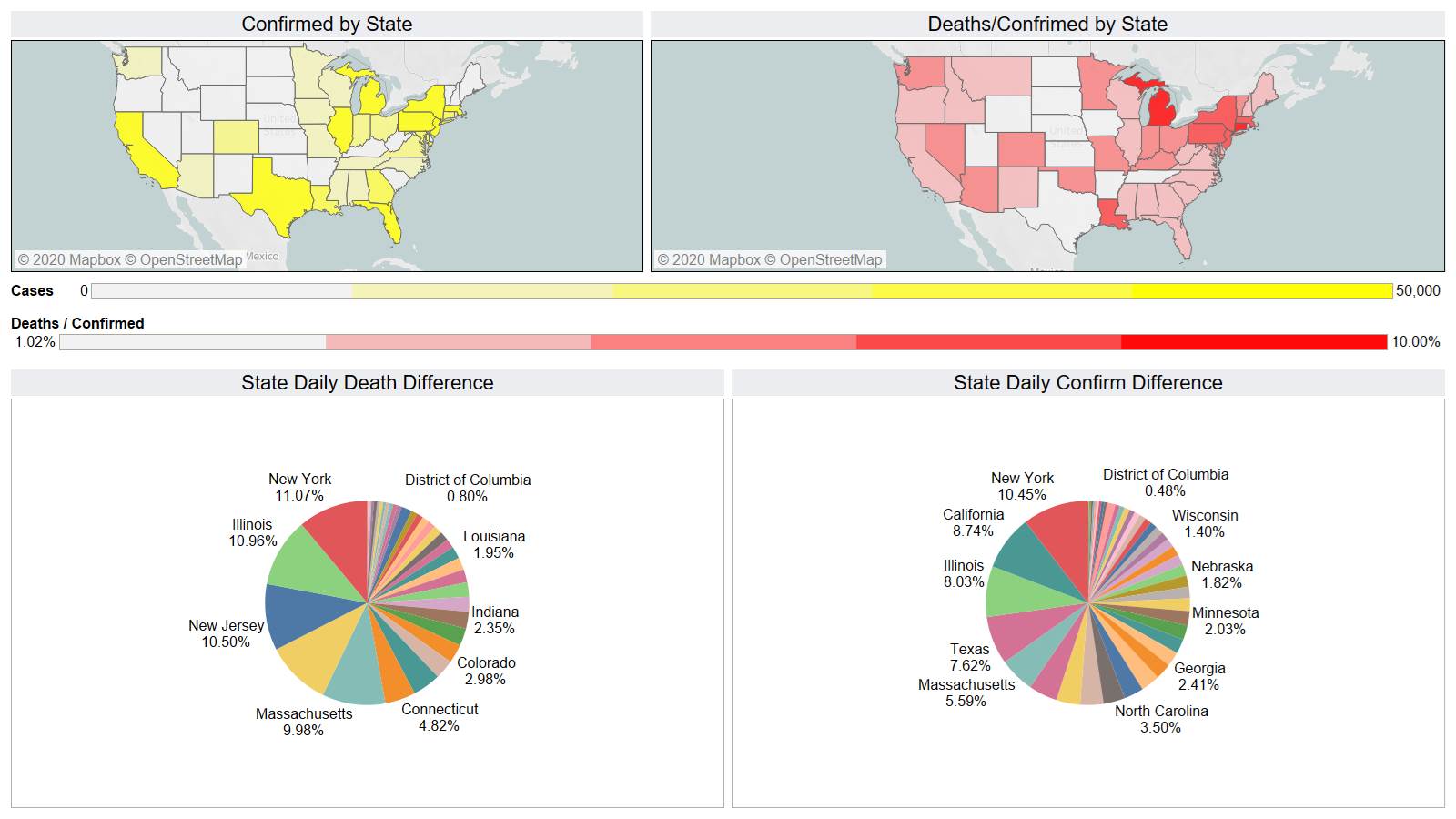
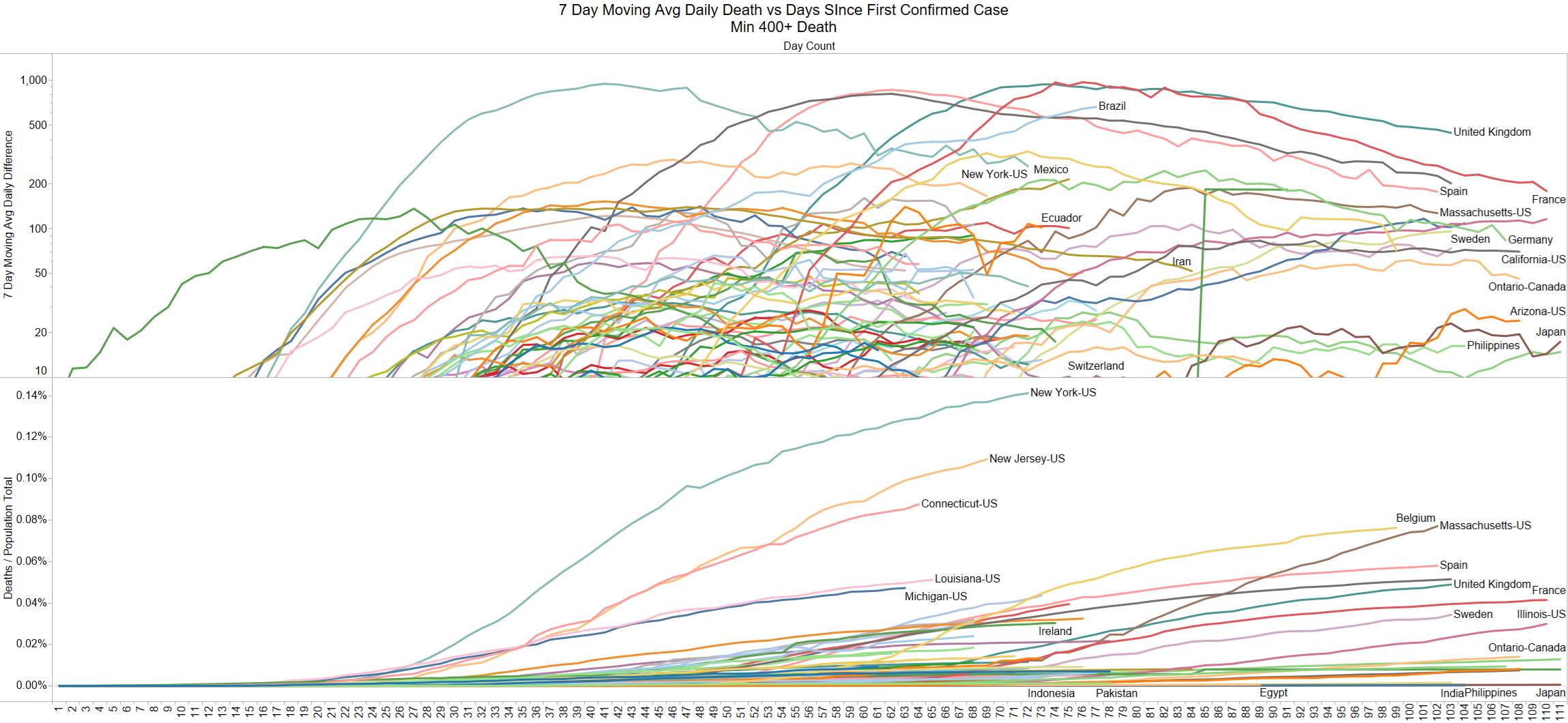
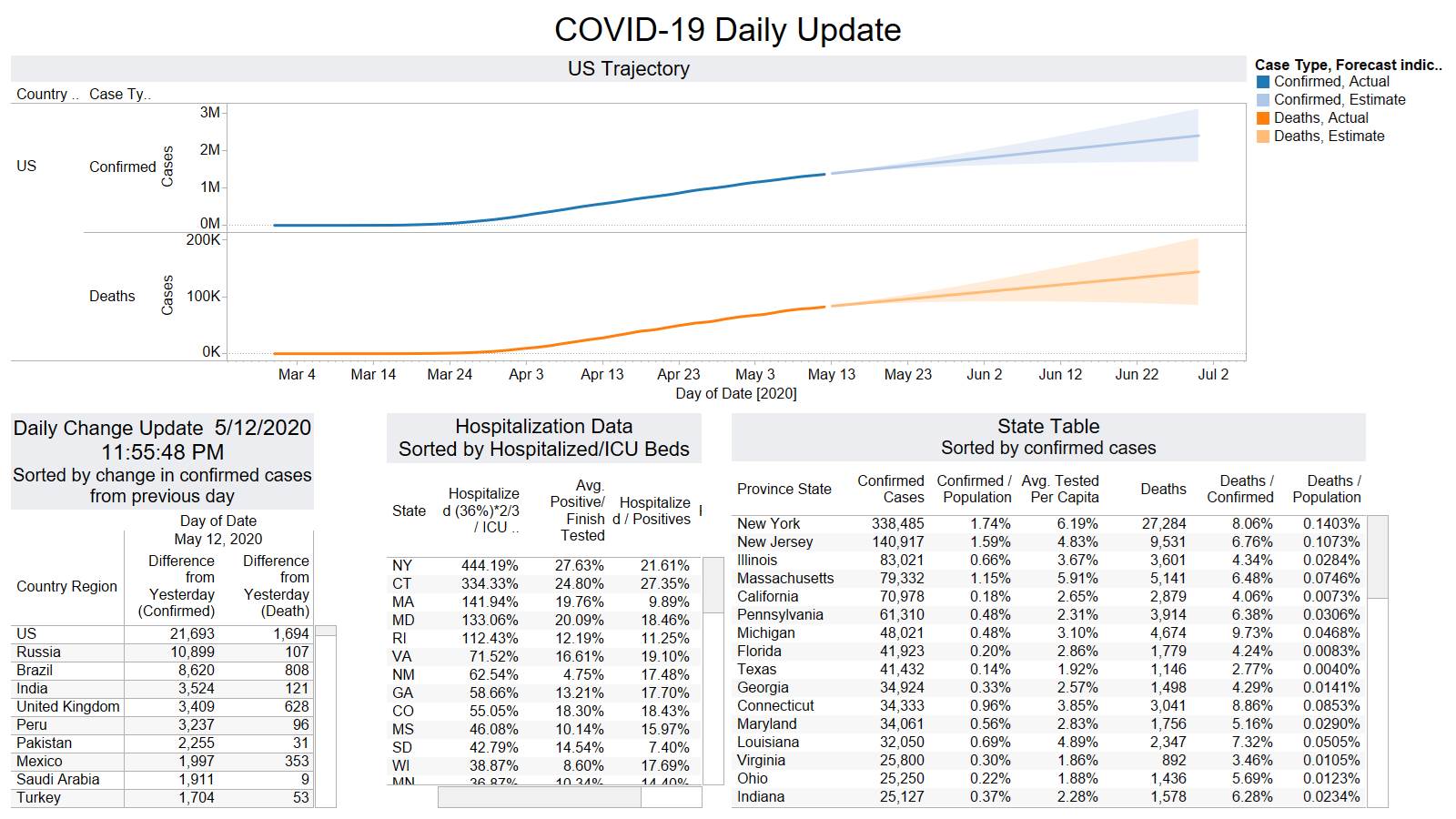
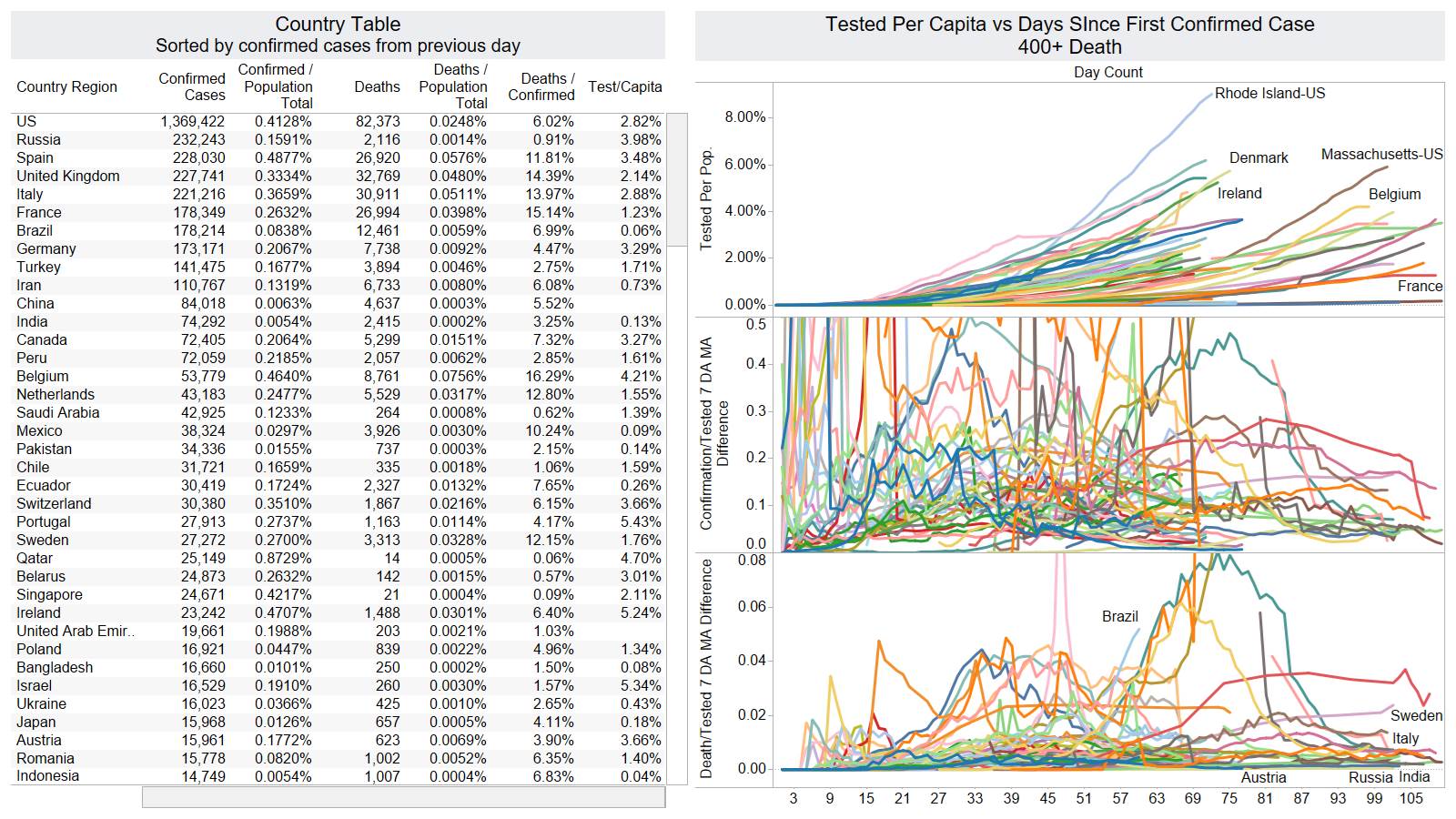
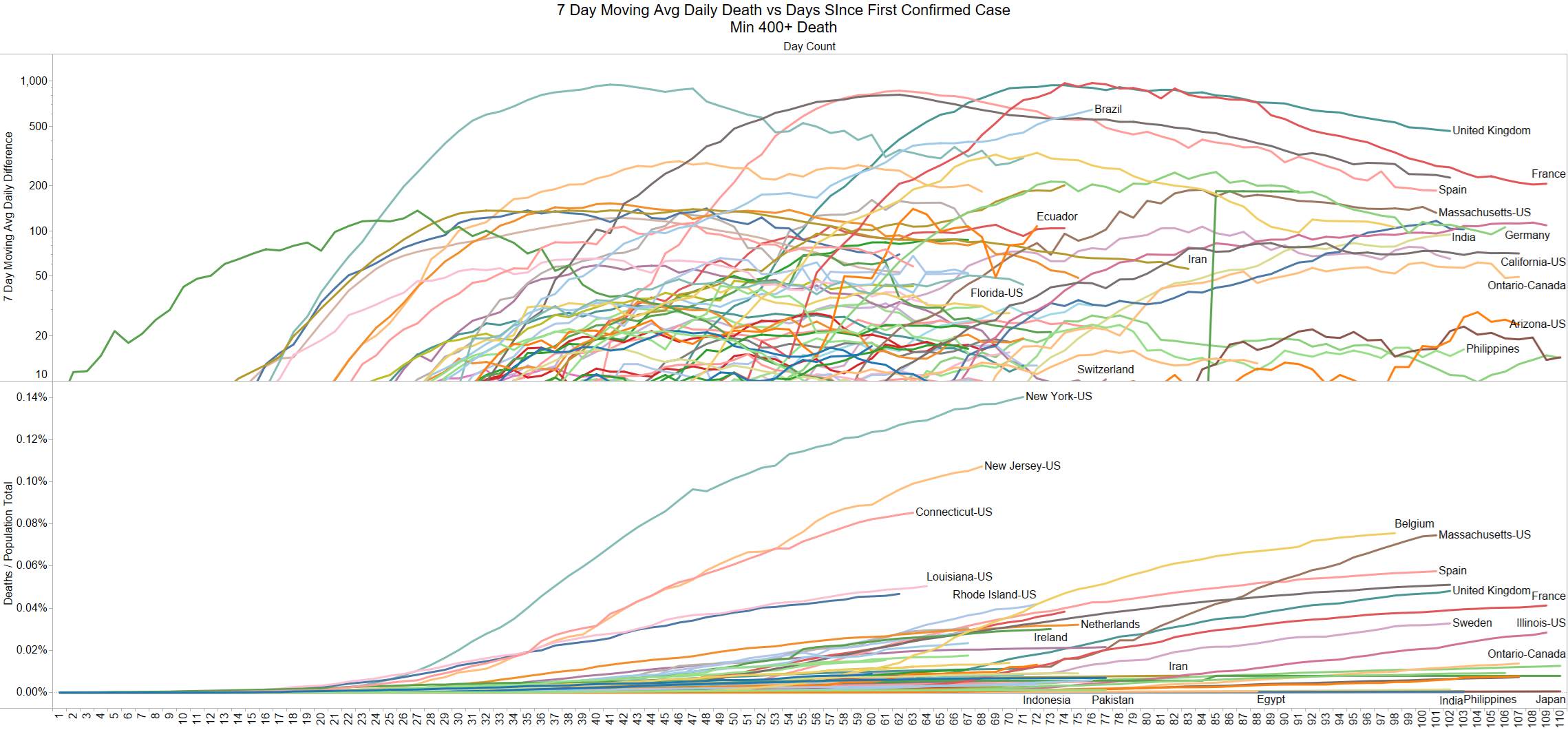
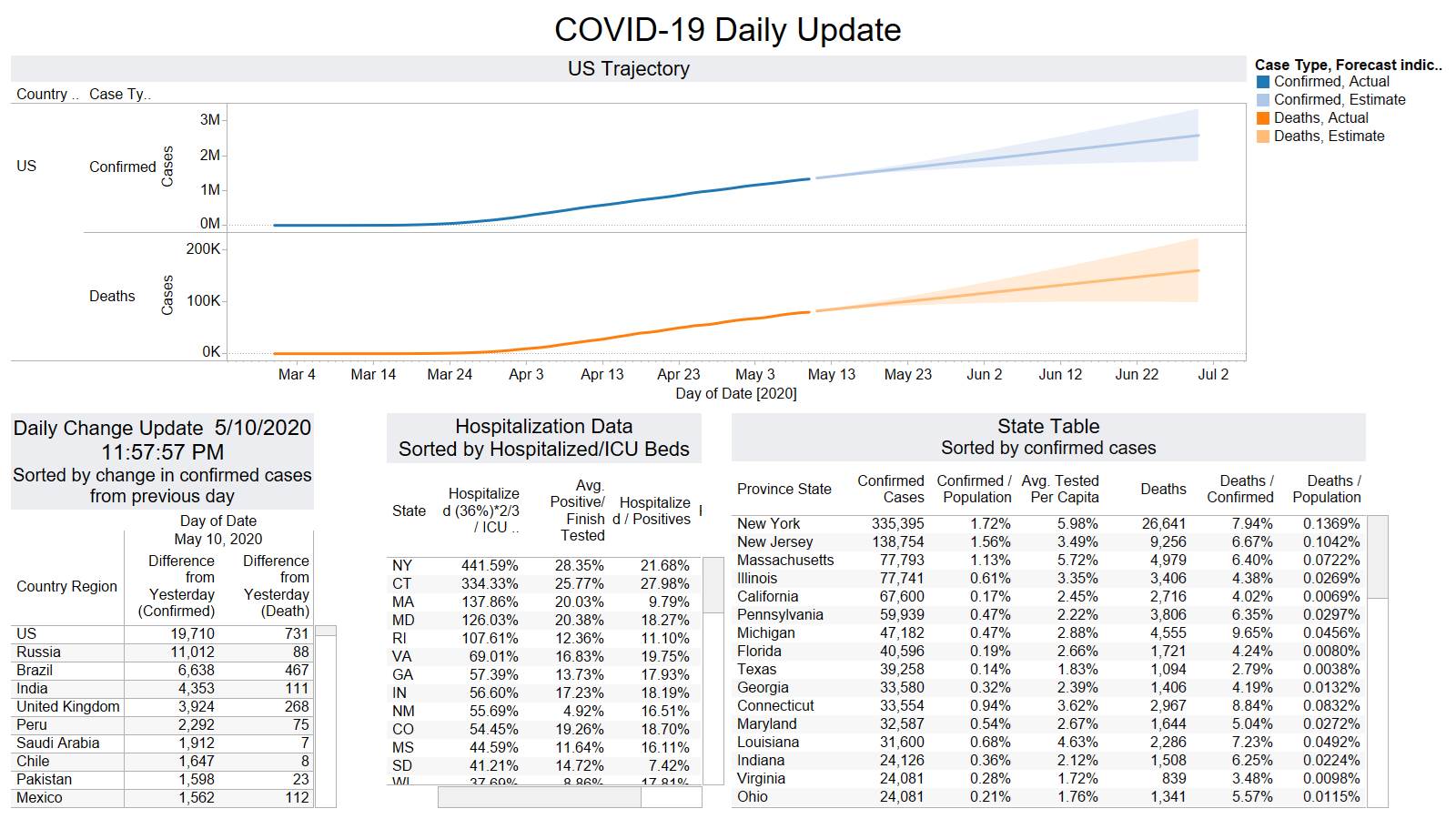
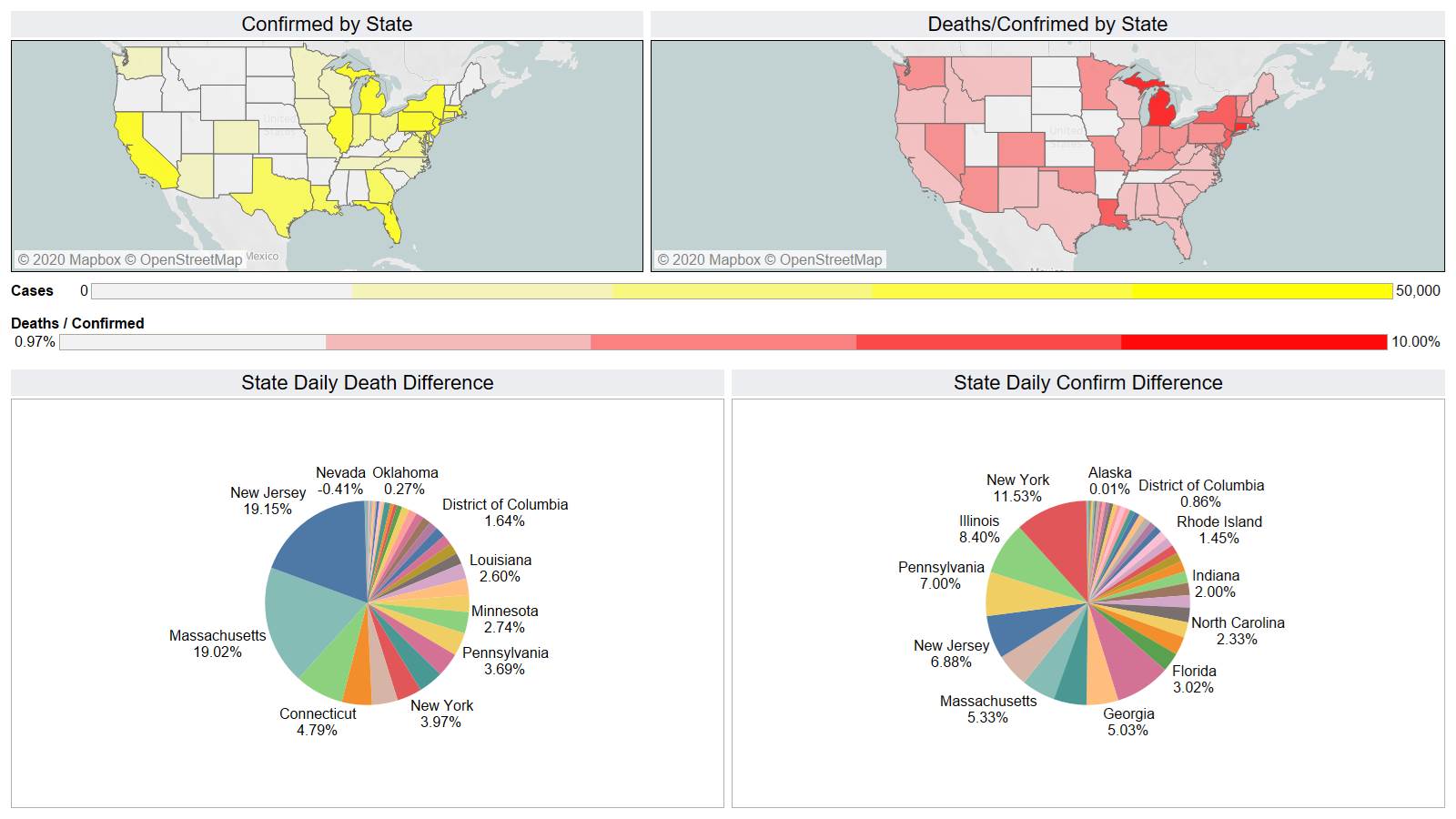
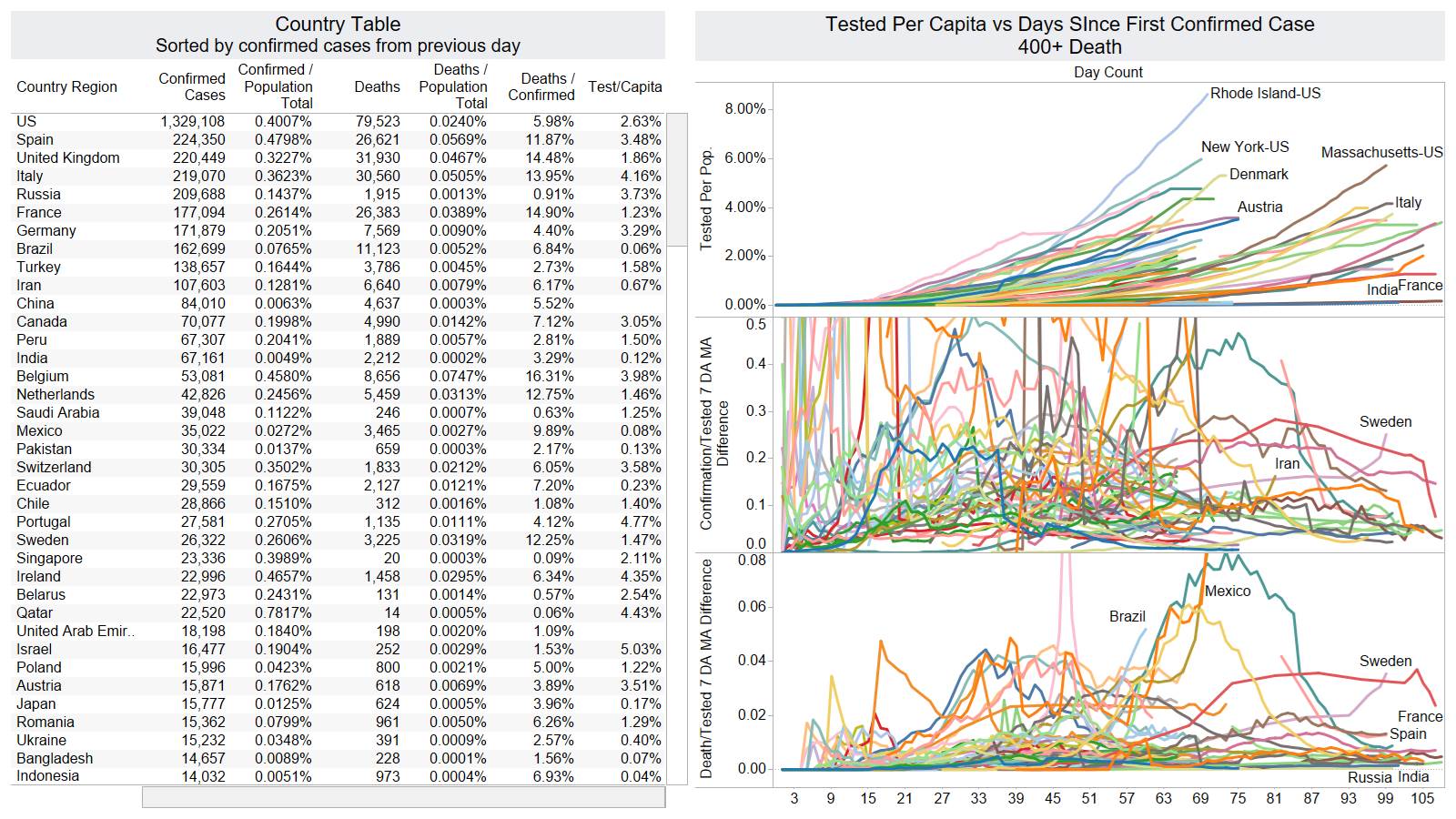
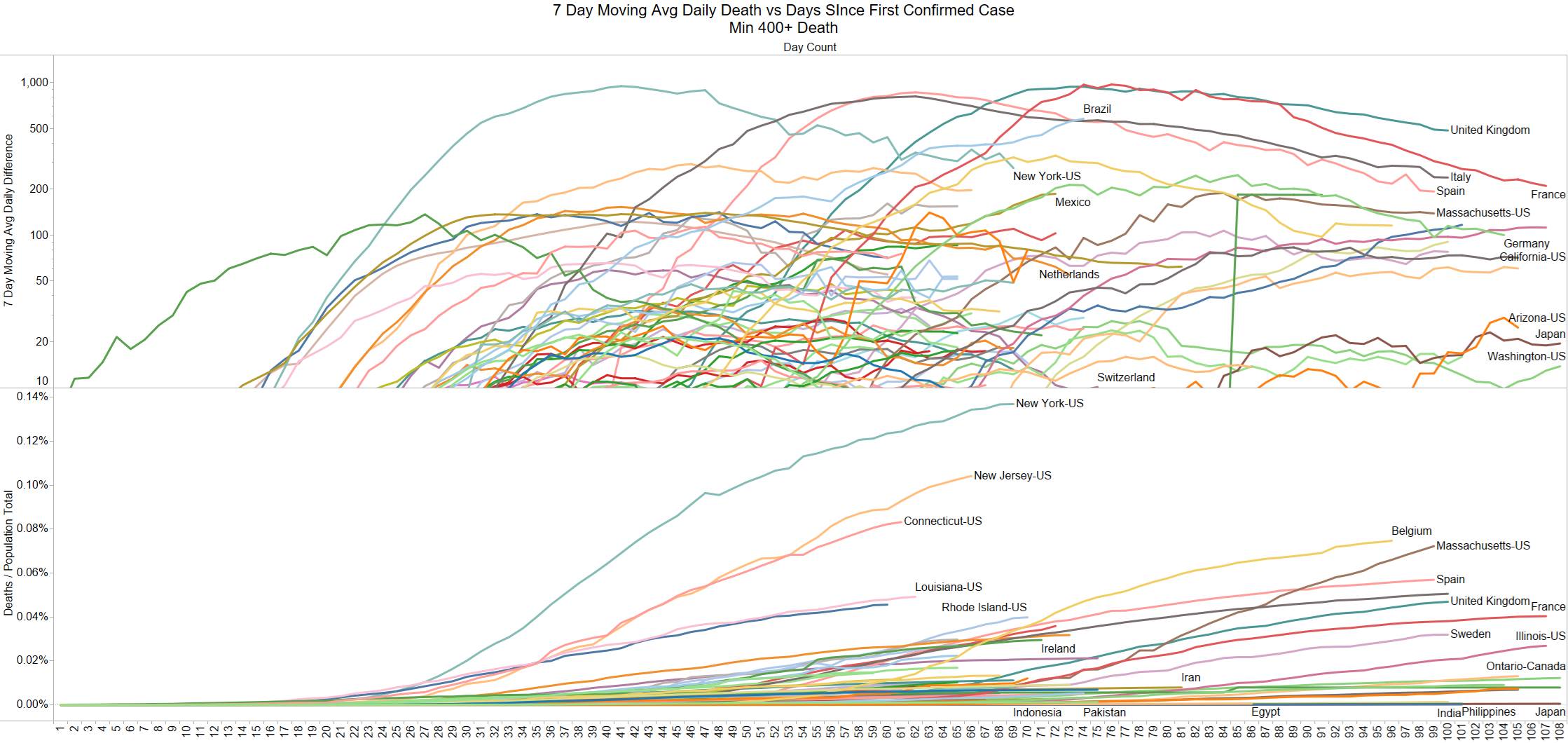
Well the good times end – with US deaths back up 1574 – and Brazil not far behind 1130
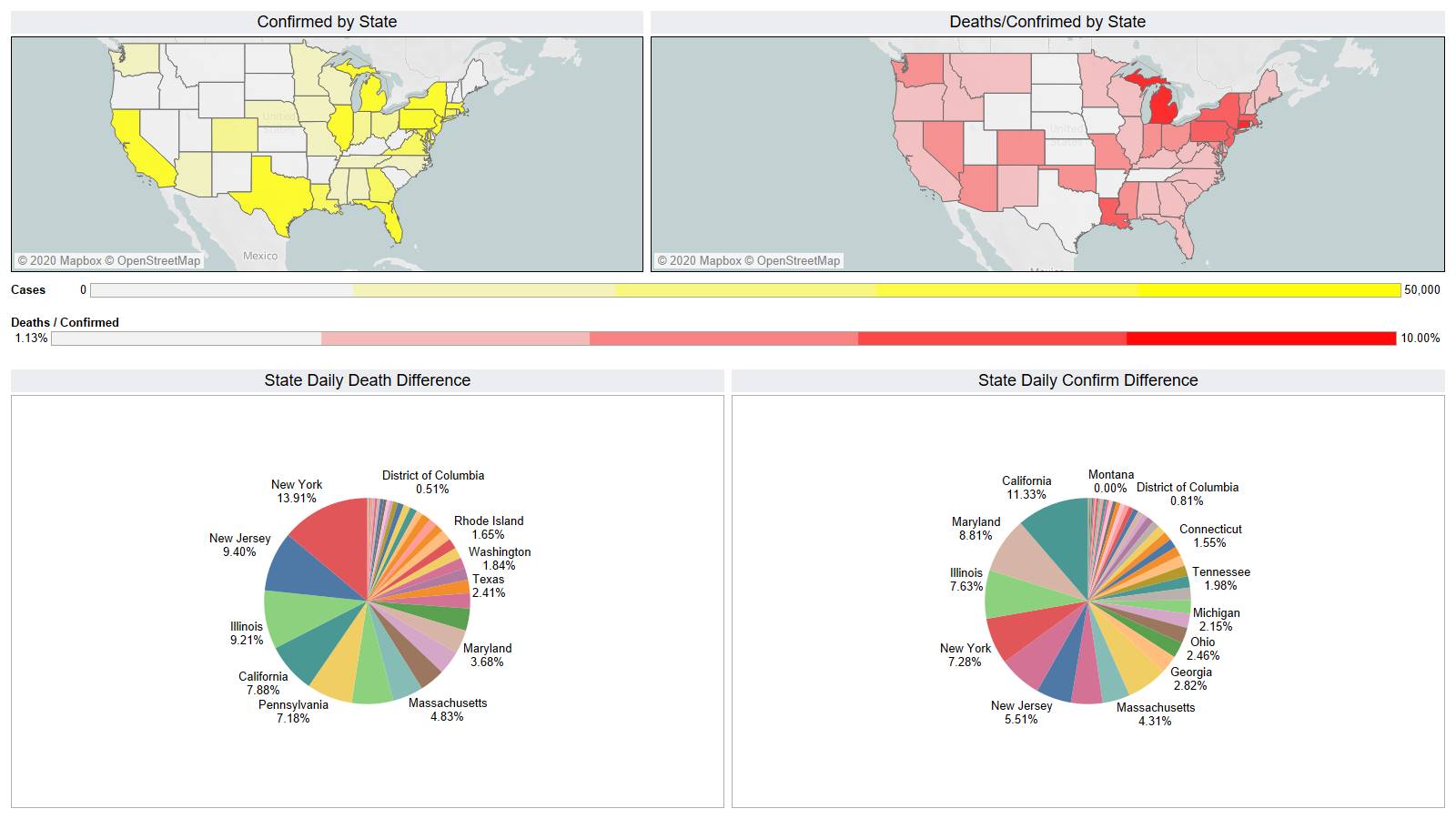
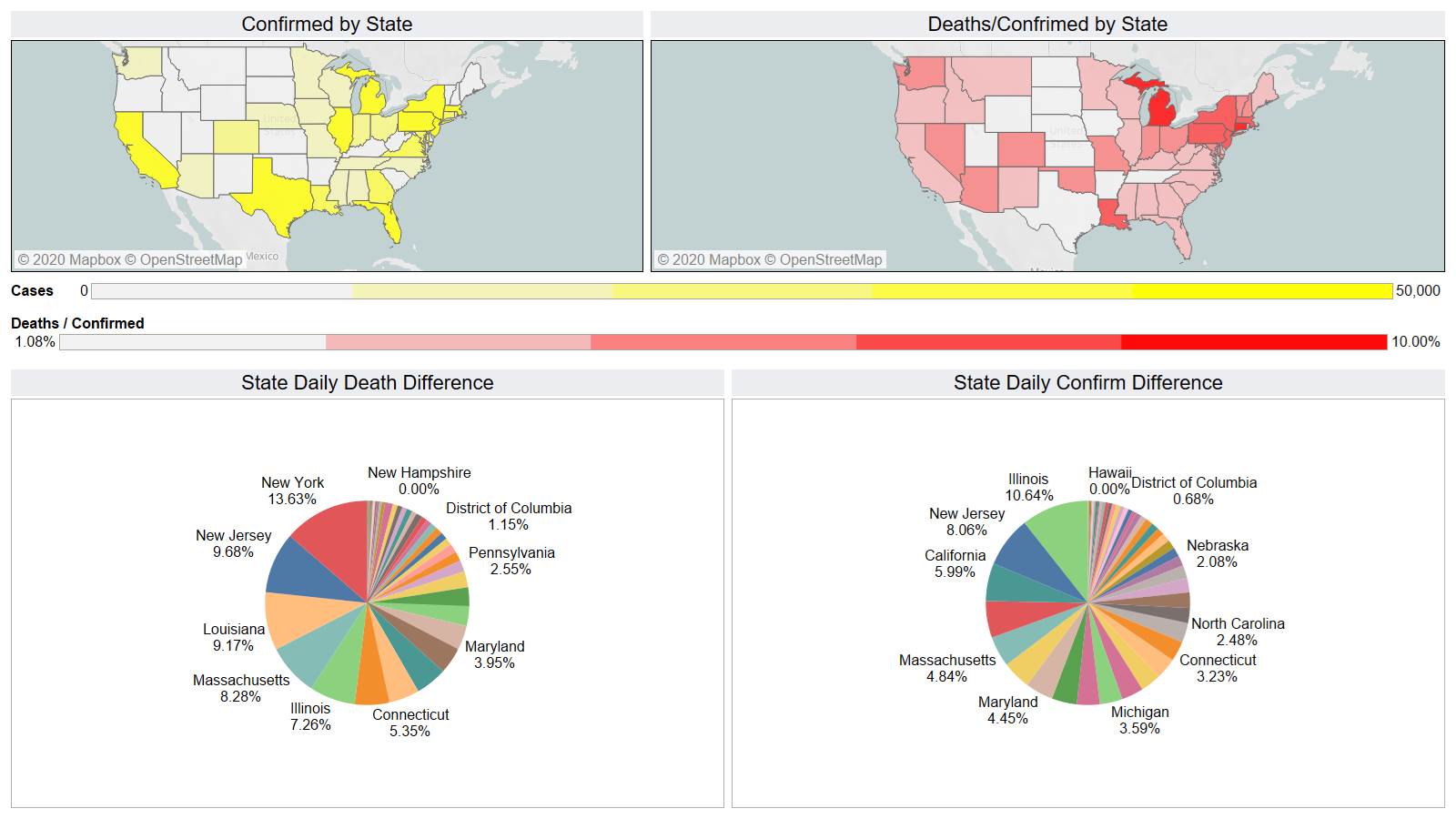
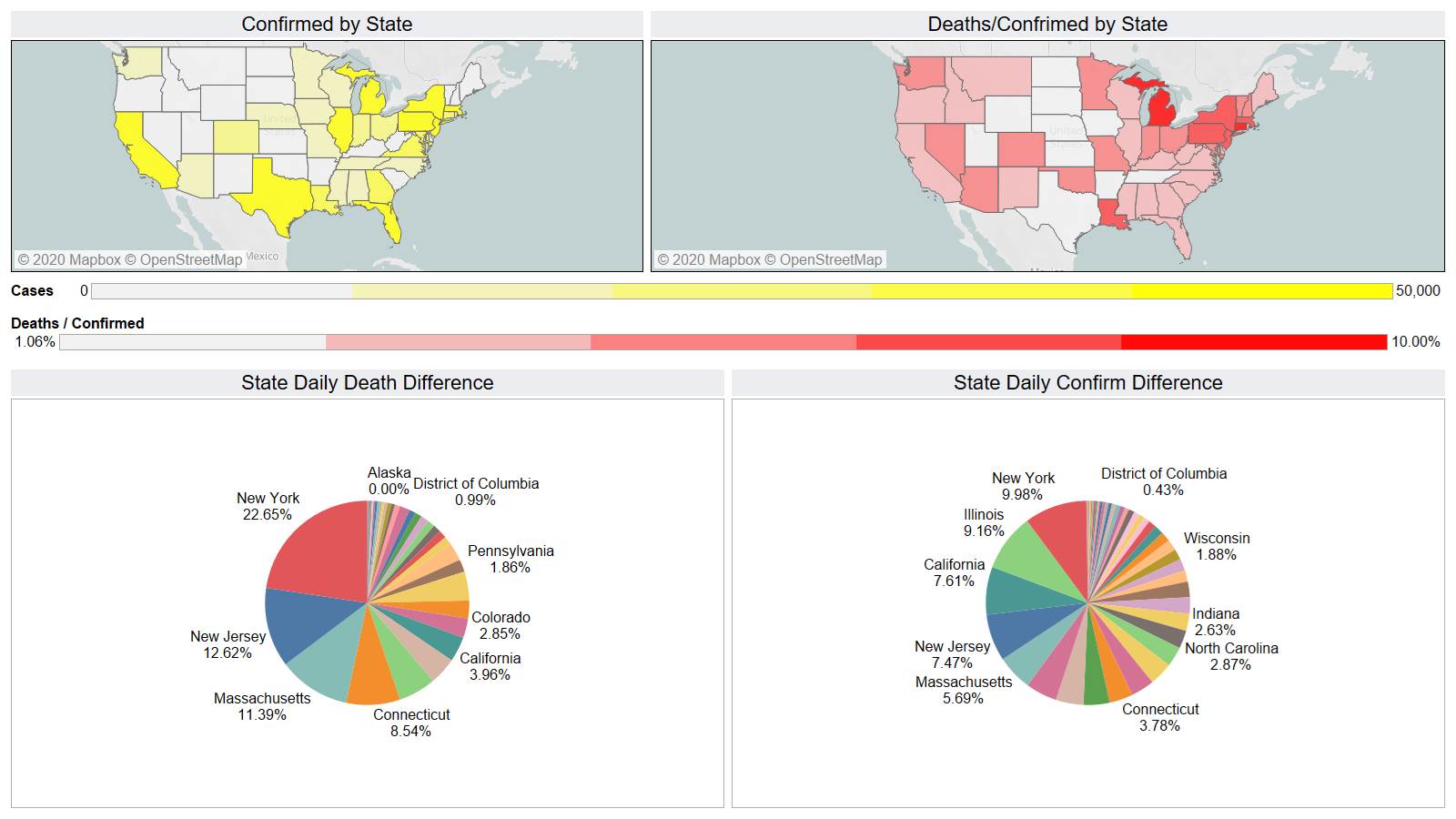
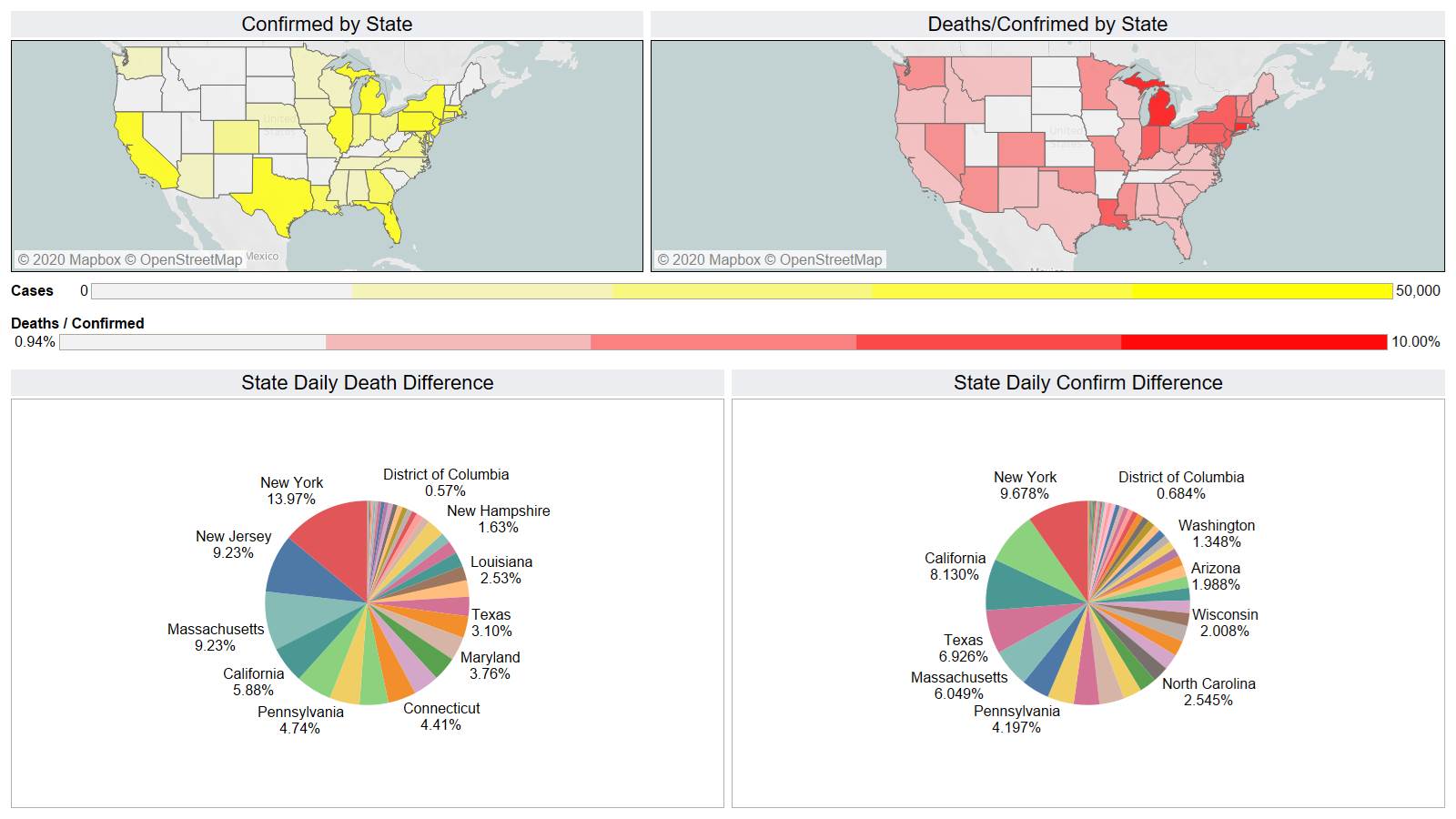
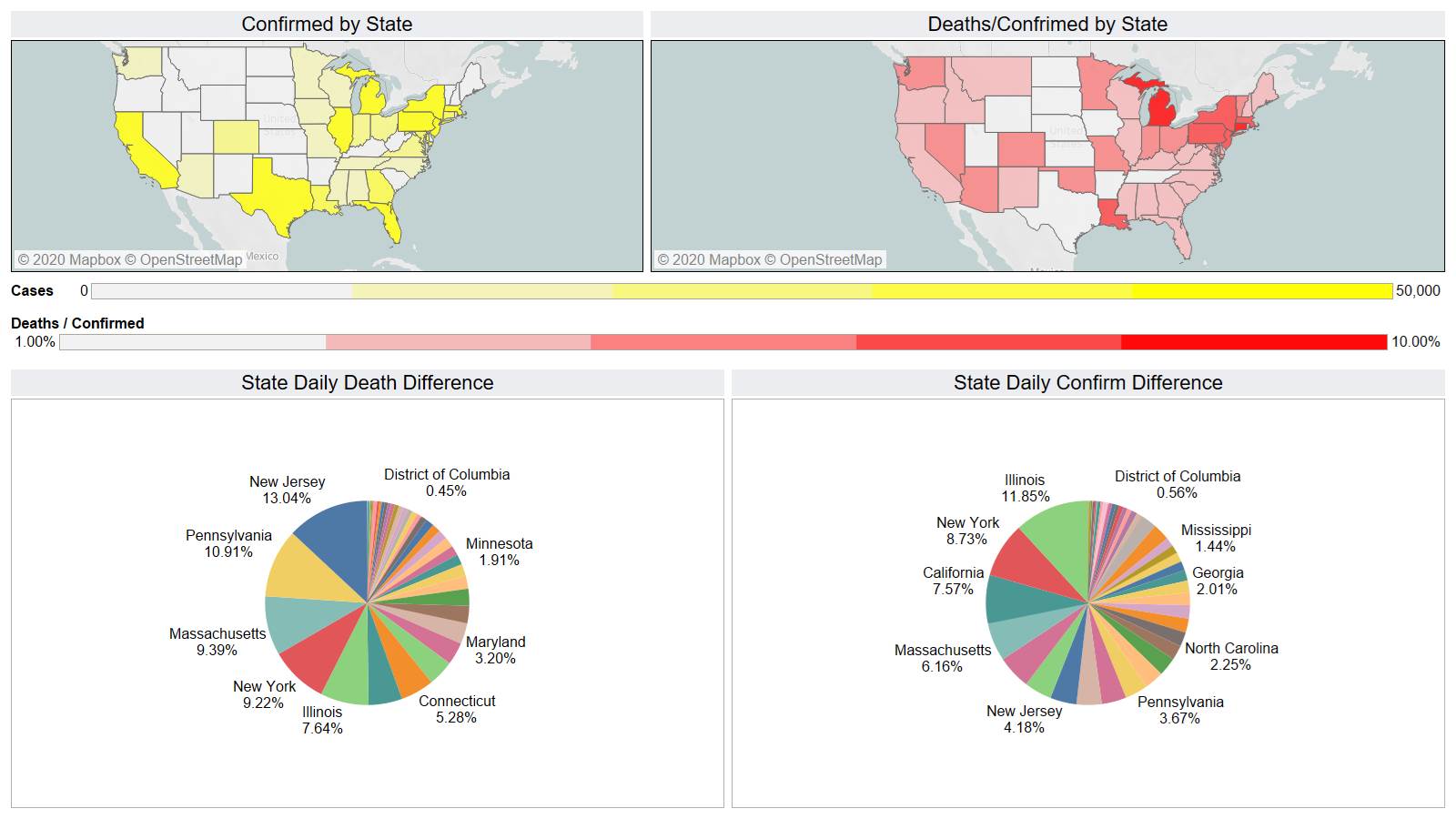
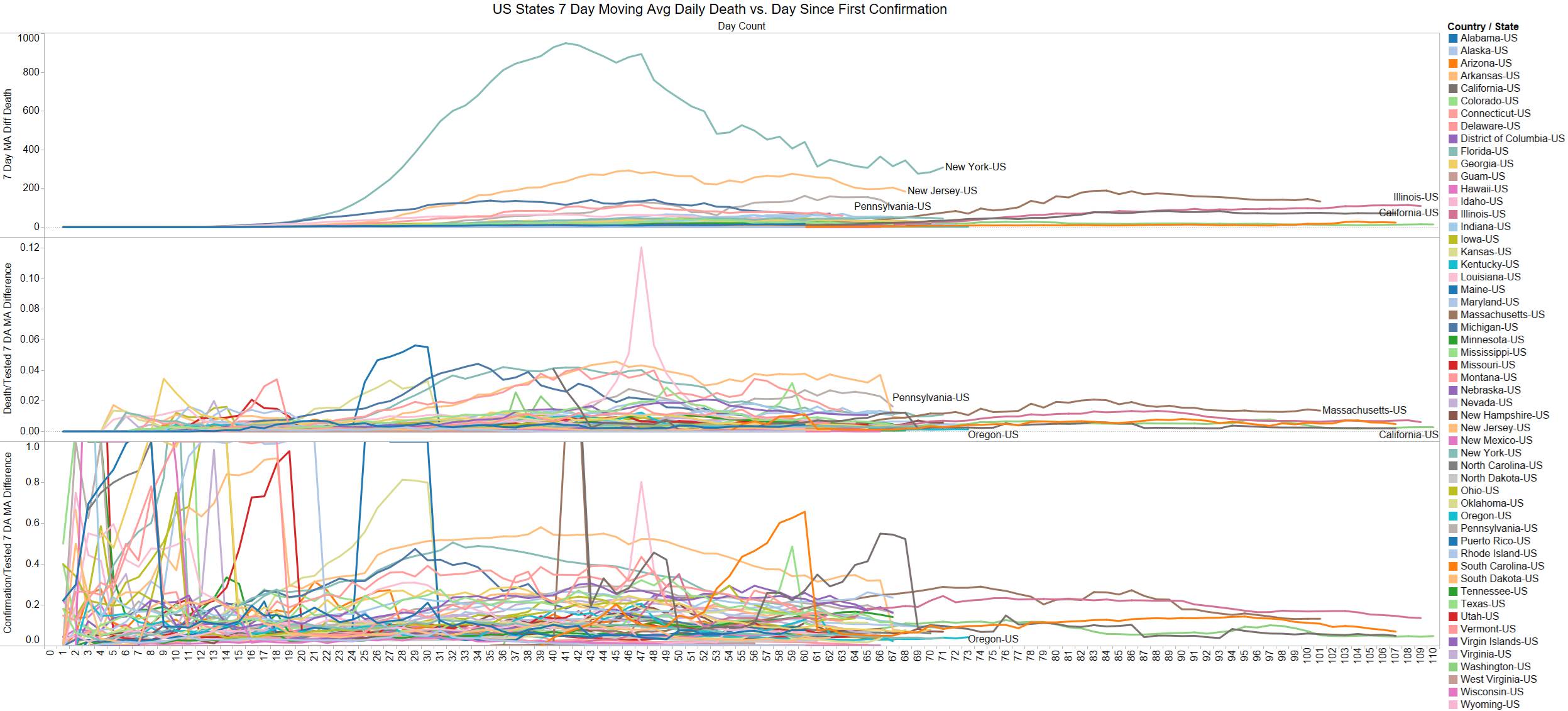
NY leading the way at 219
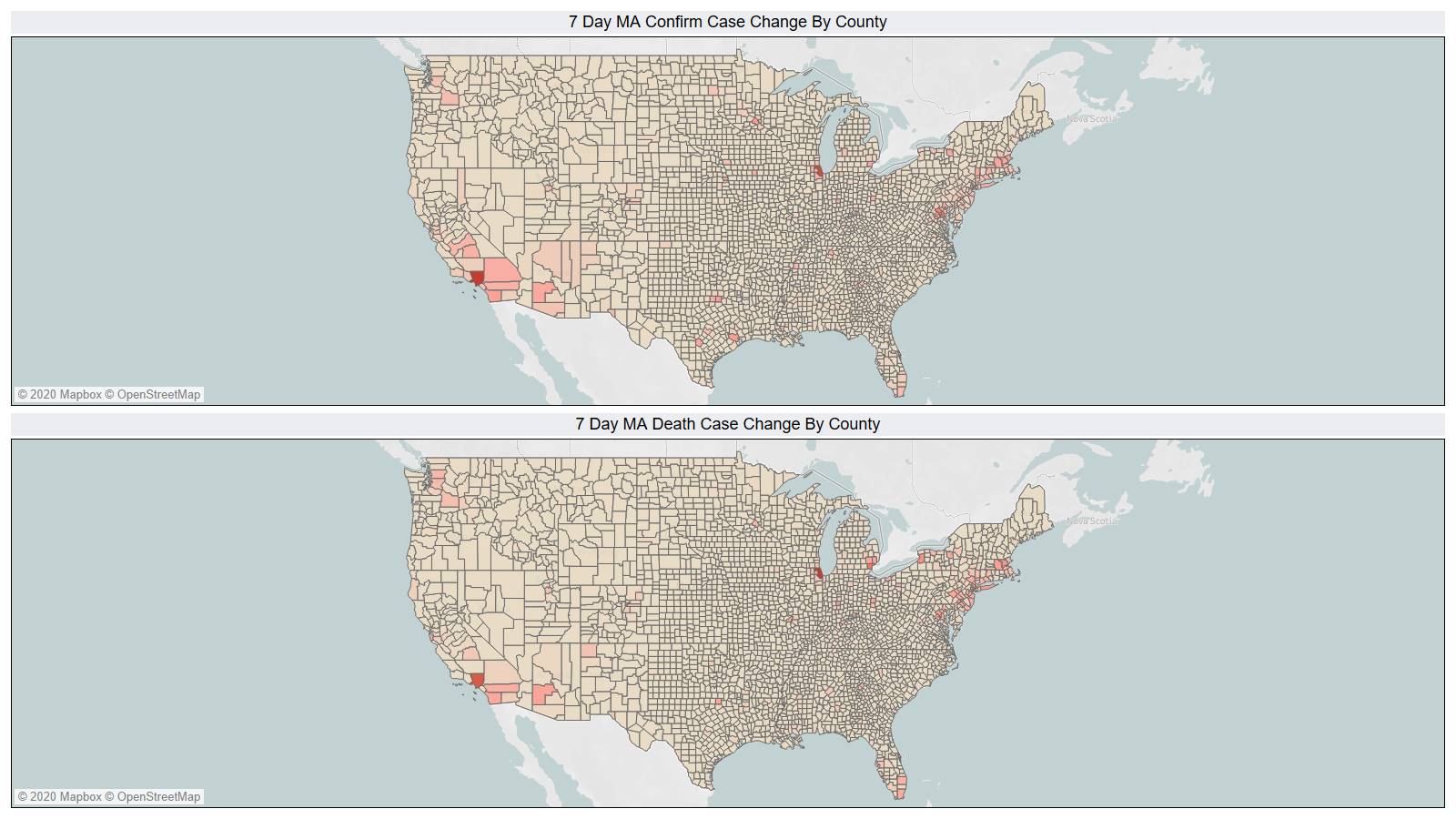
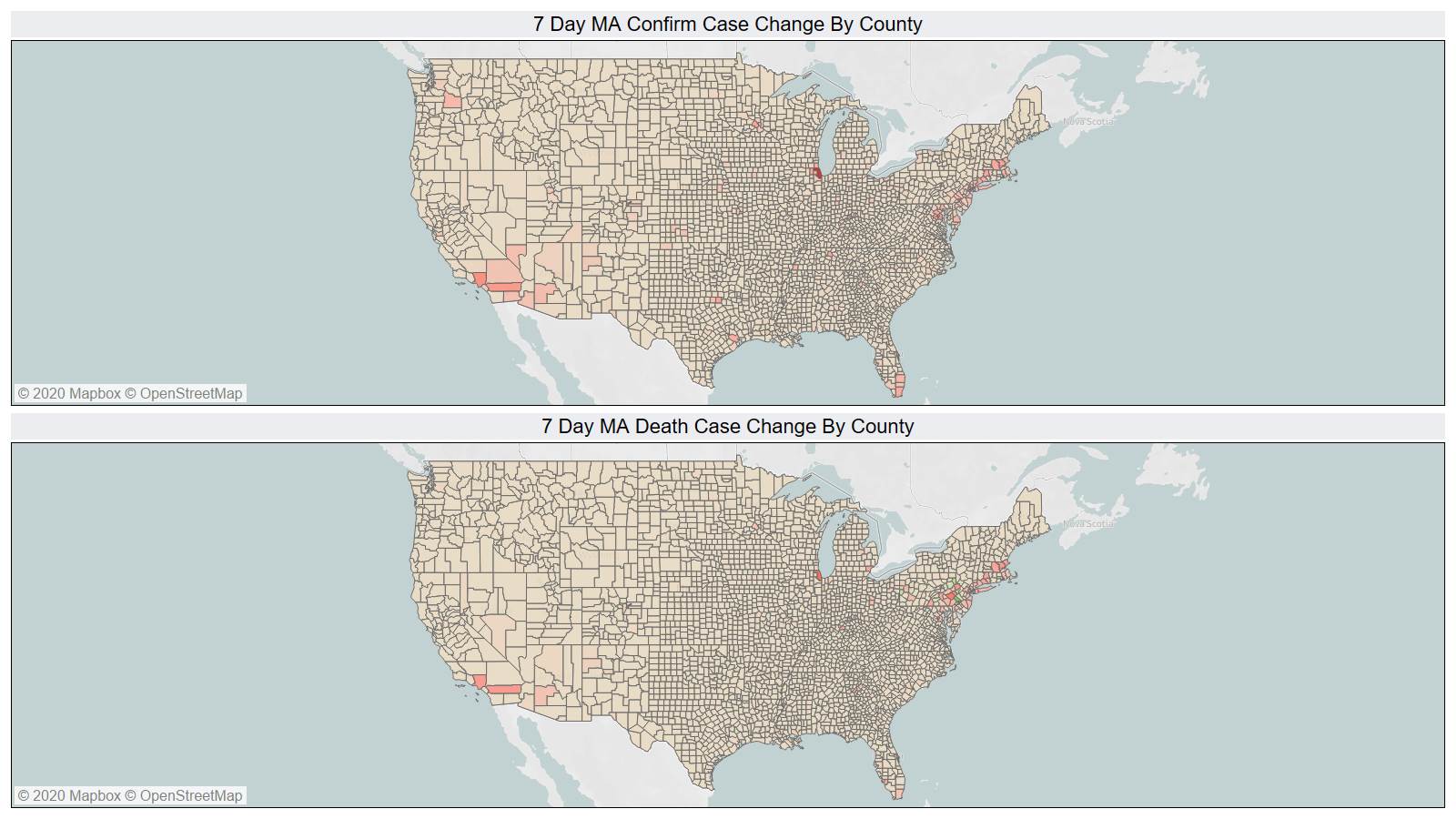
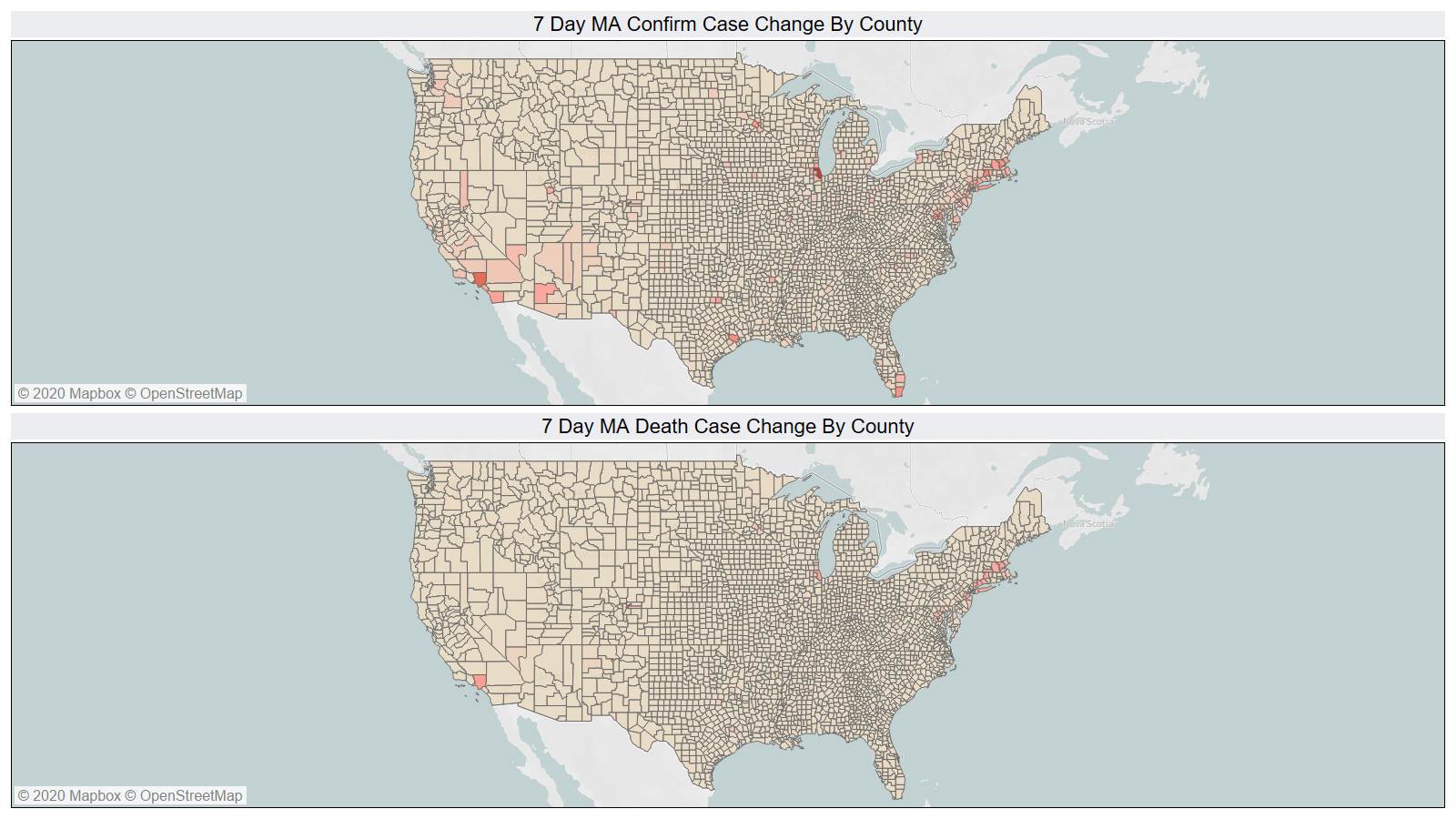
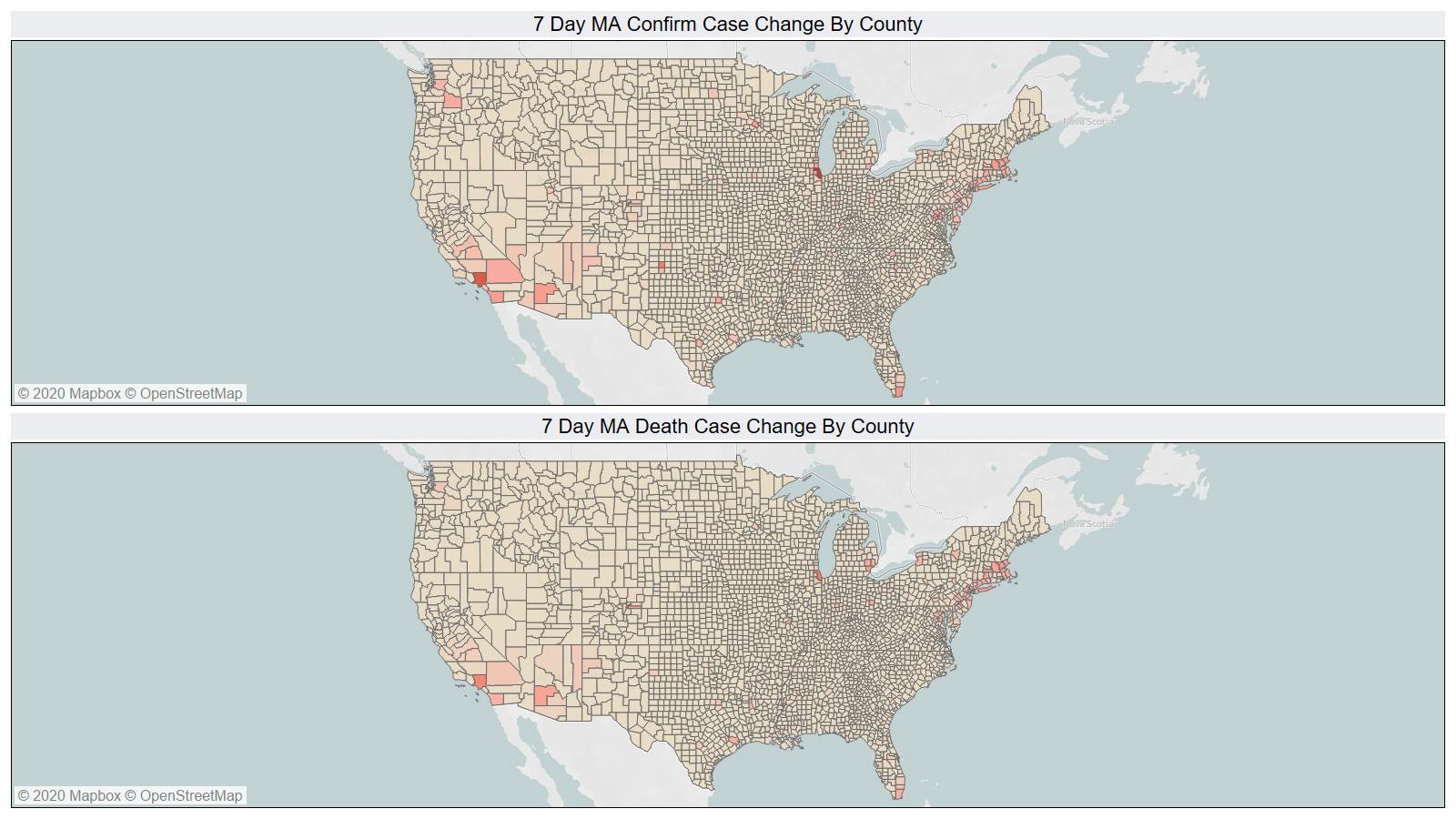
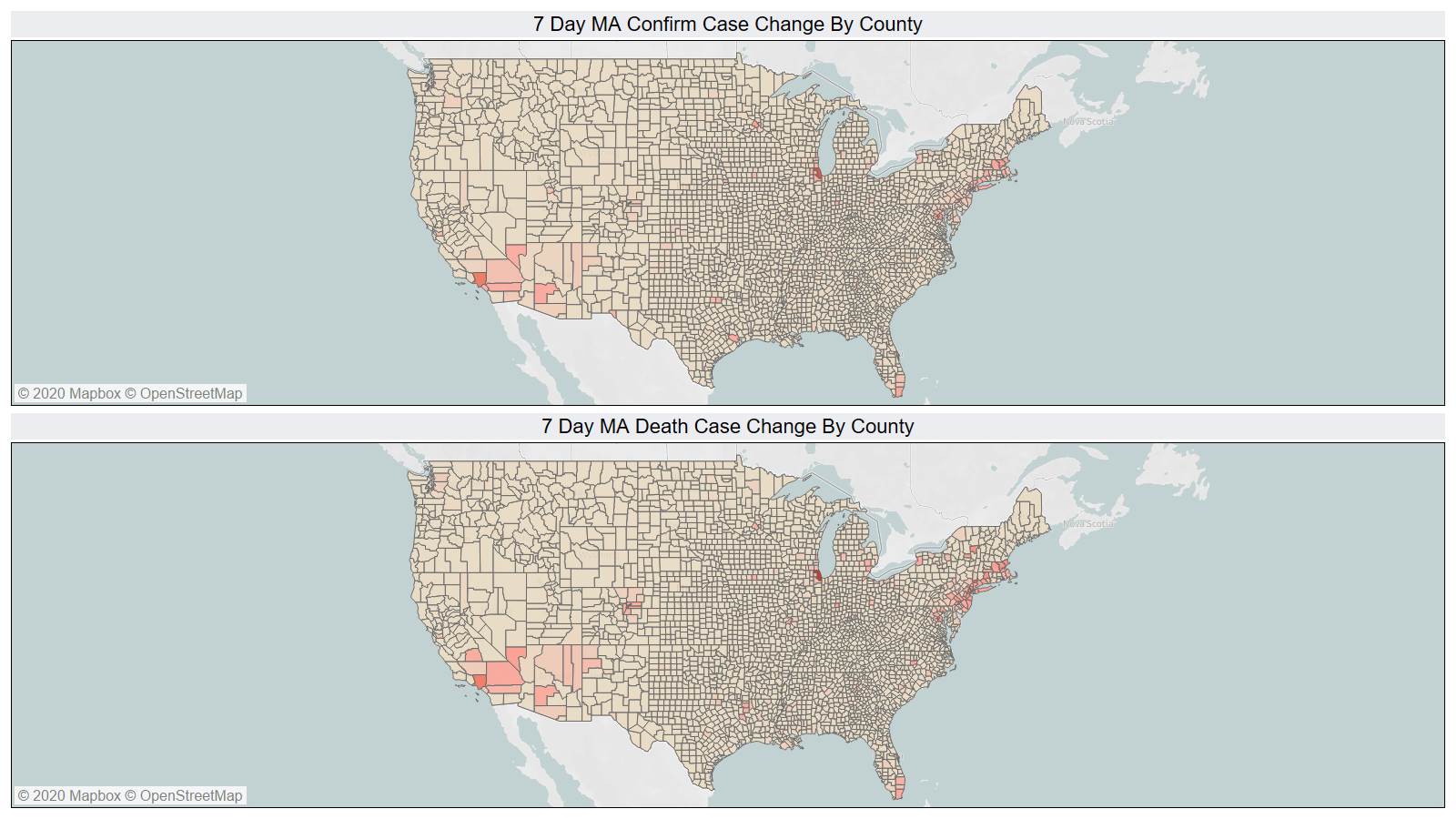
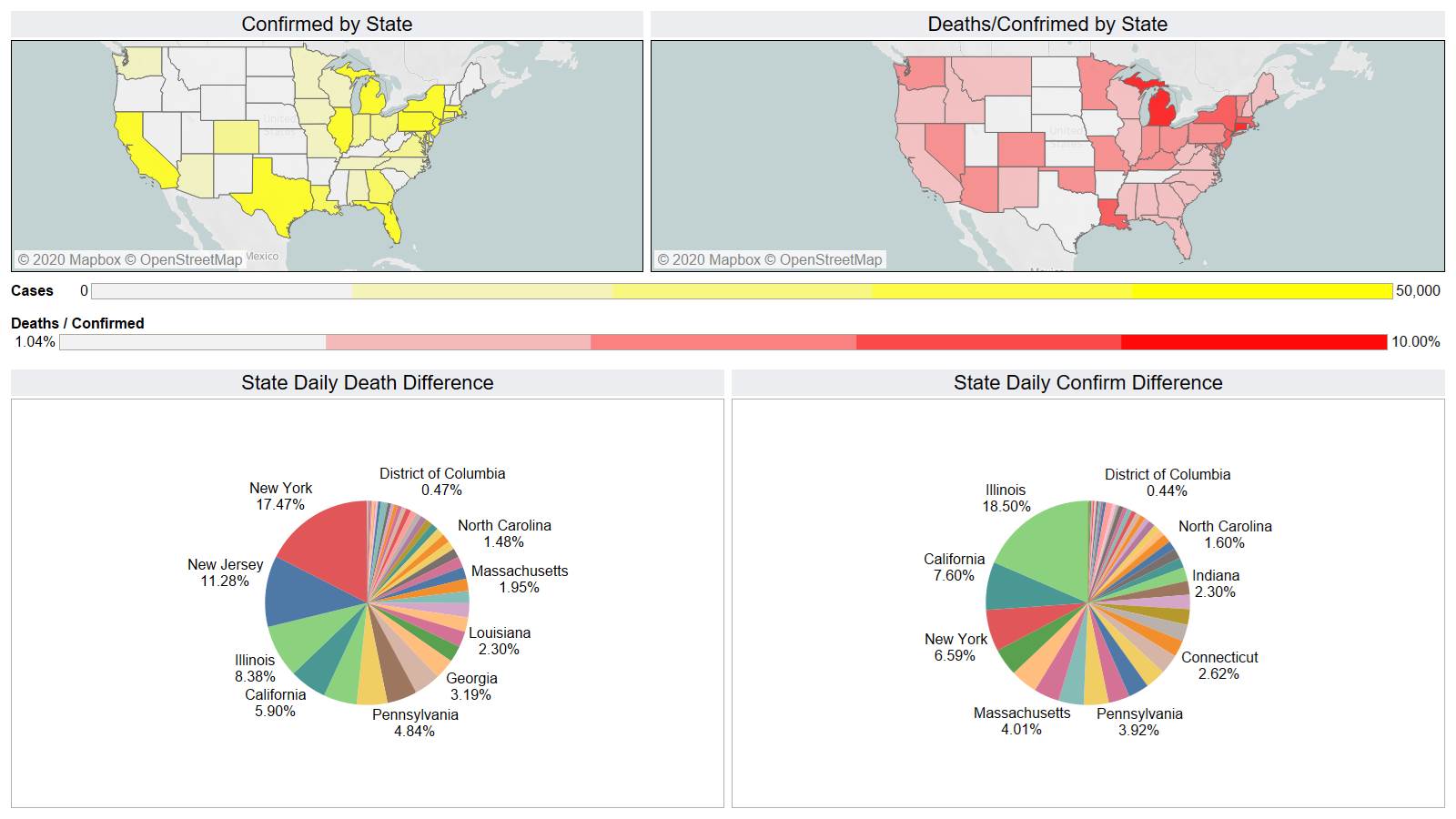
On a county level NY is not sticking out relative to Los Angeles County CA and Cook County IL.
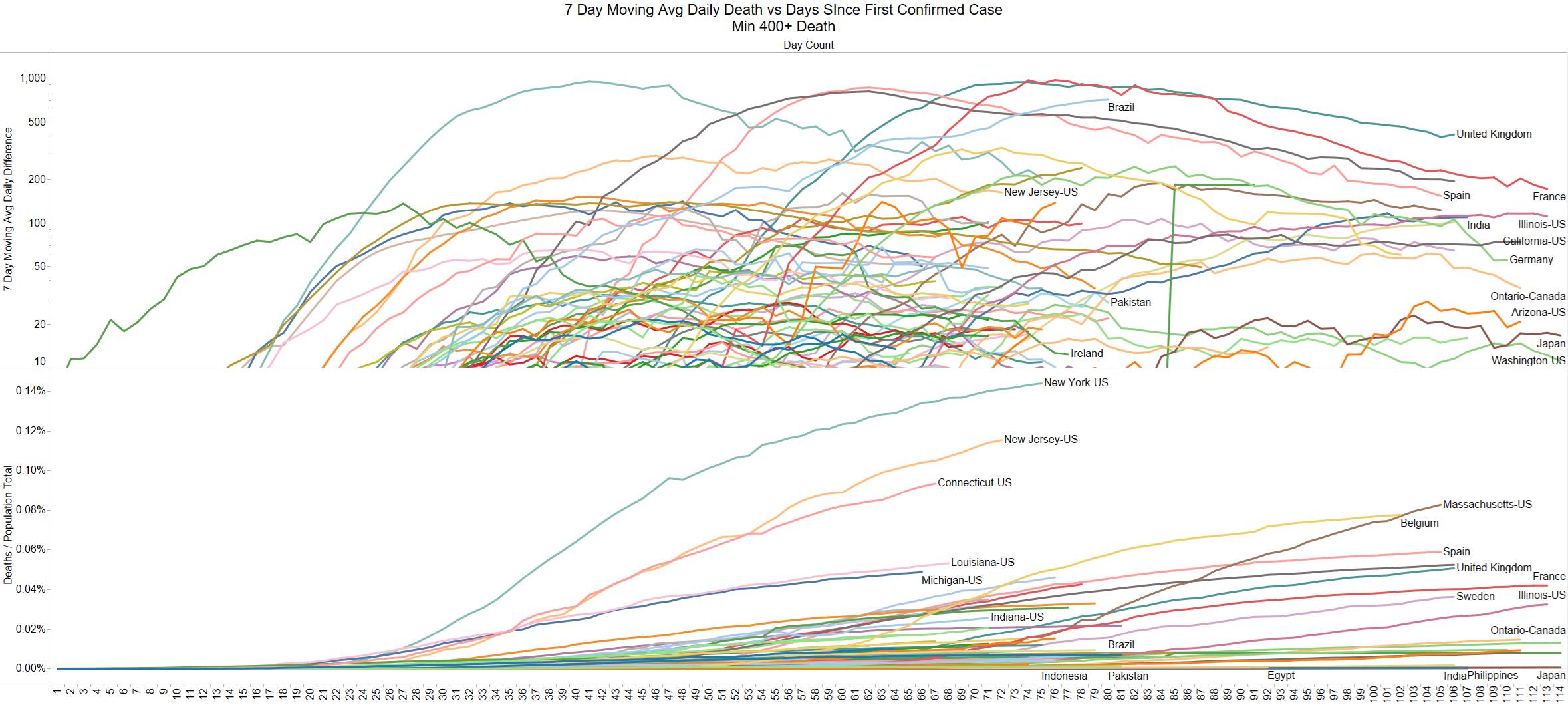
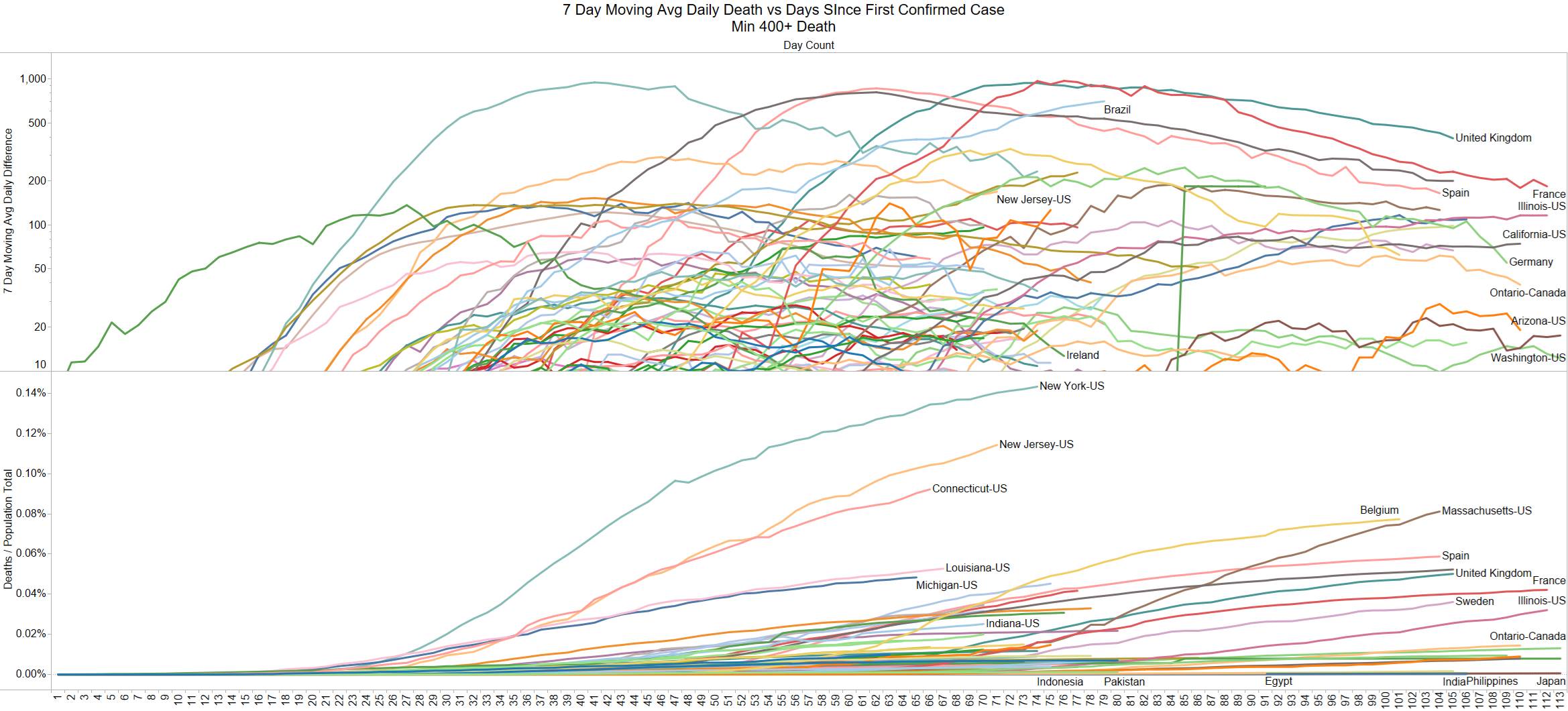
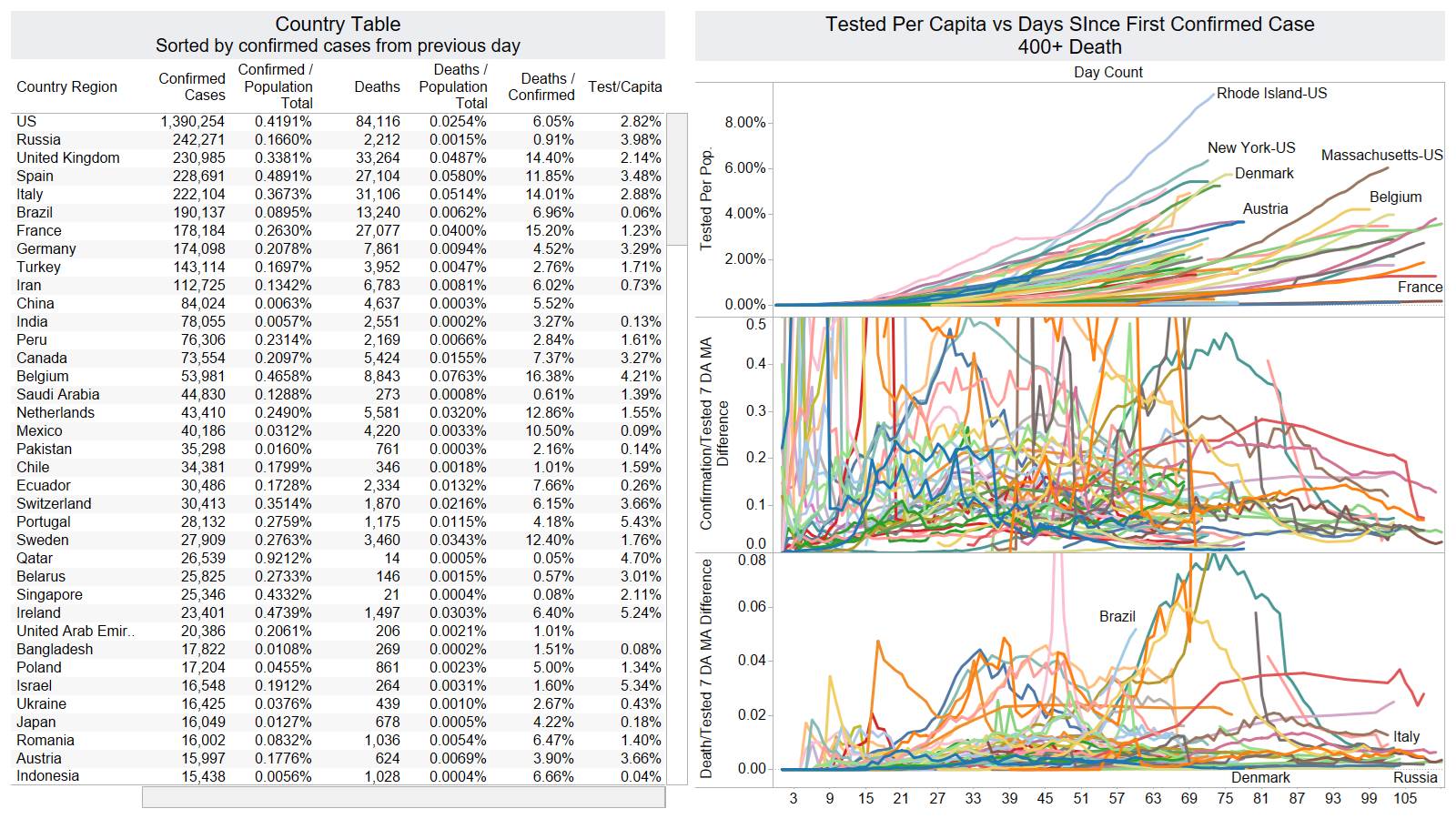
Looks like a revision to France.
Brazil is still growing in death rate. Mexico perhaps is flattening out.